
Distribution of Cellulite in the Gluteal Region
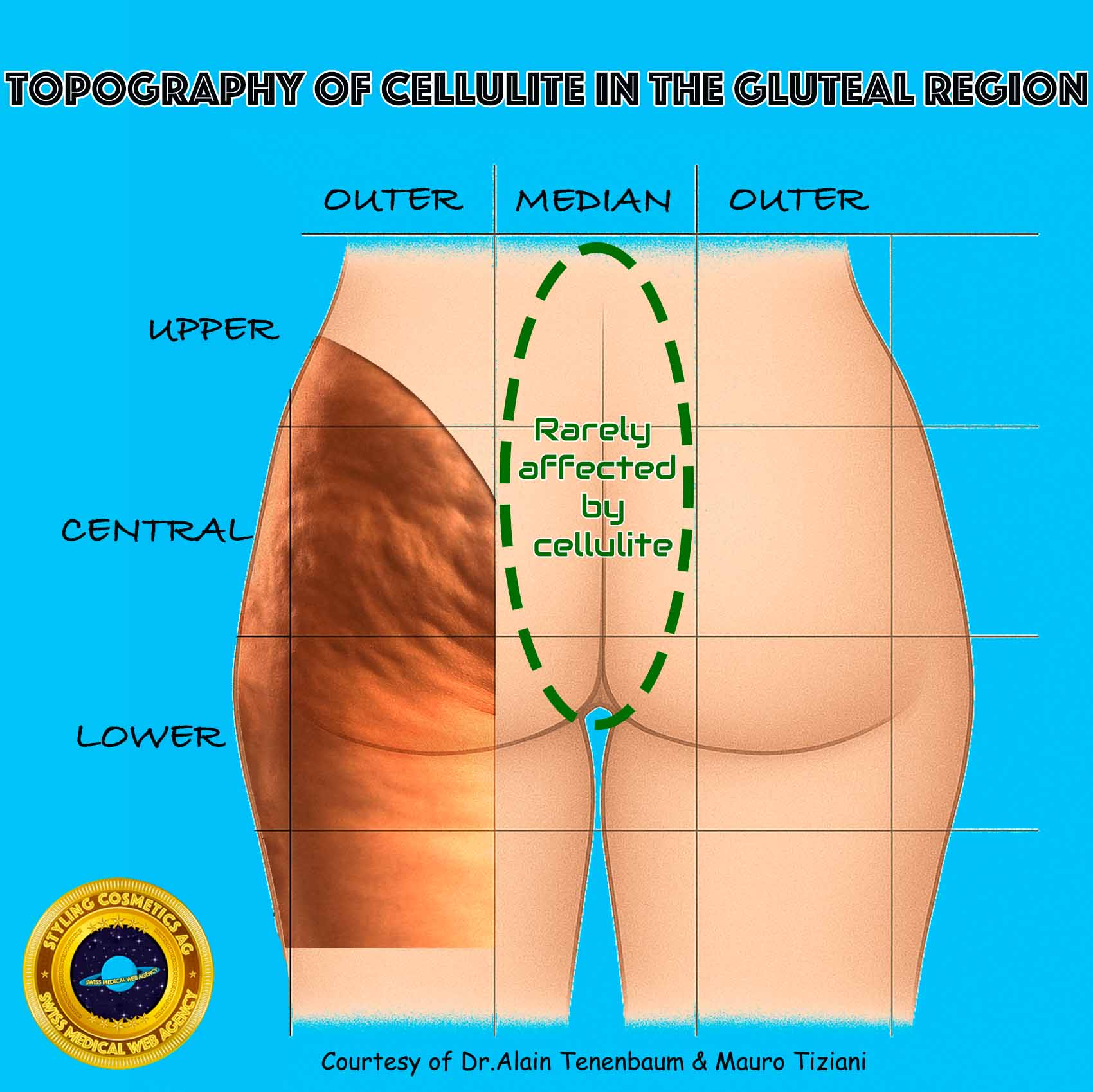
Cellulite shows a non-uniform distribution within the gluteal region. Specific quadrants are consistently predisposed to alterations of the dermis–subcutis interface, whereas other zones remain unaffected or are only sporadically involved. Recognizing this topographic pattern is fundamental prior to assessing the clinical relevance of Endopeel interventions on the gluteal area.

Areas commonly affected

- Superolateral quadrant (upper outer buttock, near the hip)
→ Typically most involved; contains numerous vertical fibrous septa and is subject to mechanical compression. - Inferolateral quadrant (lower outer buttock, close to the thigh junction)
→ Often shows visible dimpling, especially when standing. - Central buttock area (mid-portion)
→ May be affected, though usually less than outer quadrants. - Subgluteal fold (“banana roll”)
→ Transition zone between buttock and thigh, where fatty deposits are frequent and cellulite can accentuate folds or bulges.
Areas rarely or never affected
-
Medial quadrant (toward the intergluteal cleft)
→ Almost never involved; different subcutaneous tissue architecture, less tension from septa. -
Upper central area (below the iliac crest, above the gluteus maximus center)
→ Rarely affected; connective fibers more horizontal, fat layer thinner. -
Deep central buttock (over the ischial region, sitting surface)
→ Generally spared; fibrous septa less vertical, fat compressed by body weight.
Summary
Cellulite most commonly involves the outer and lower buttock regions, while the medial and central parts (near the cleft and sitting area) are almost always spared.

Biometric Considerations
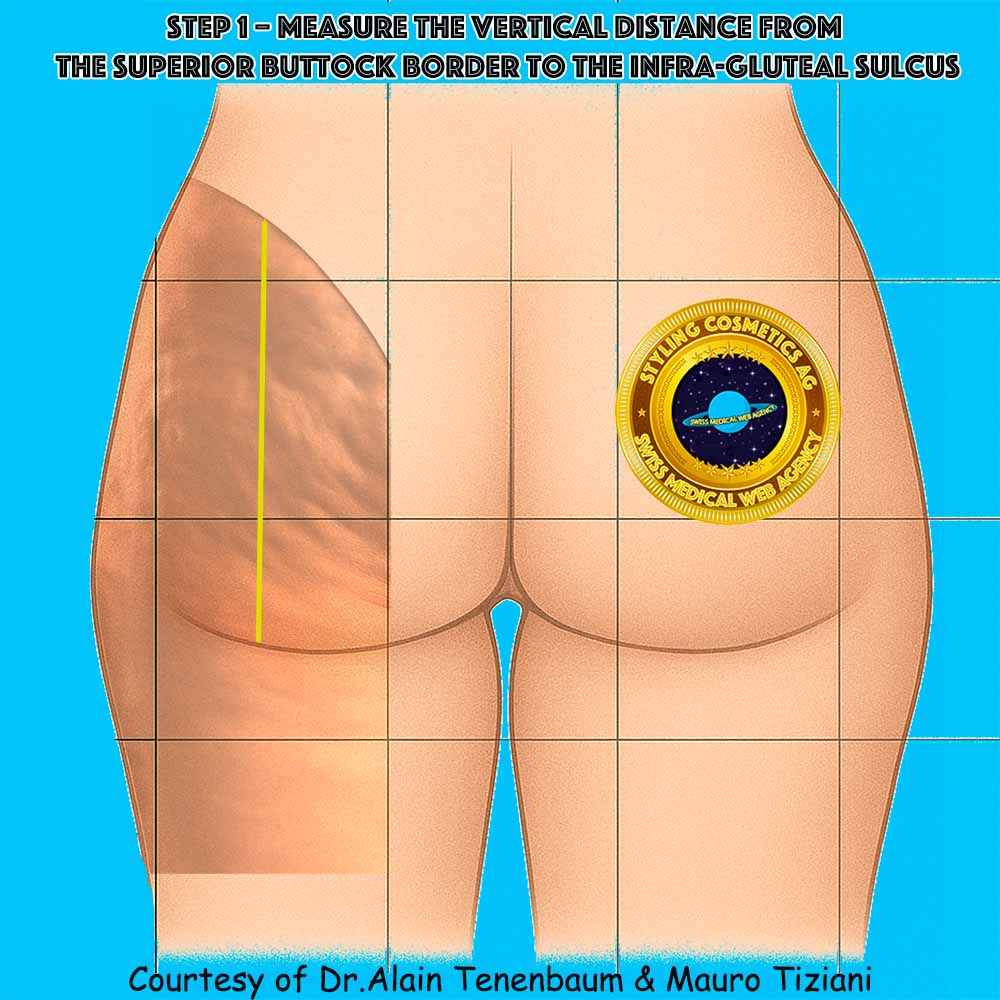
When the vertical height of the buttock is defined as 100%—from the superior border to the infra‑gluteal sulcus—two reproducible segments can be identified. These landmarks help standardize cellulite mapping and guide targeted interventions.
Upper segment (~40%)
-
Extends from the superior buttock border to the horizontal line passing through the inferior apex of the presacral triangle.
-
Useful as a reference for marking and for anticipating less pronounced dimpling in many patients.
Lower segment (~60%)
-
Extends from the presacral reference line down to the infra‑gluteal sulcus.
-
Encompasses the majority of visible dimpling and structural changes in typical phenotypes.
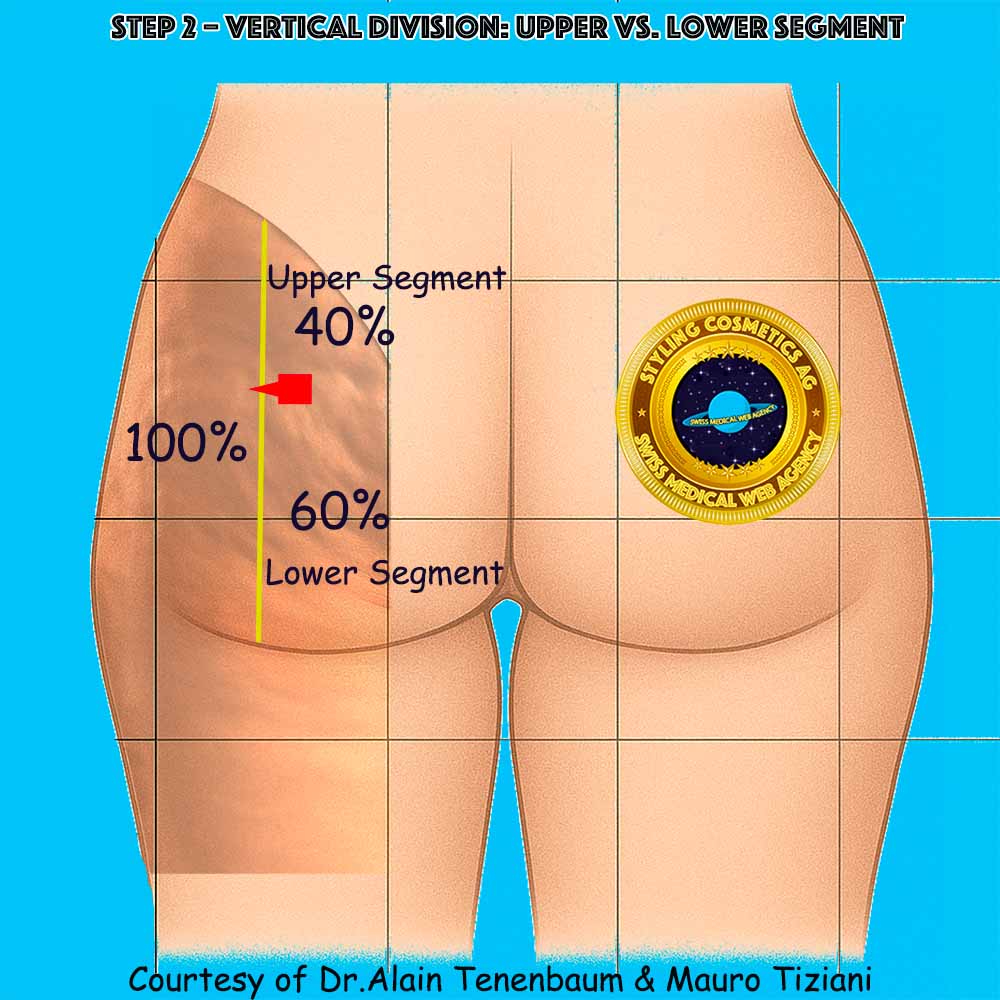
100%
Total buttock height
40%
Upper segment
60%
Lower segment
Draw the horizontal red line separating the upper and lower segments

The horizontal red line divides the buttock into upper and lower segments.
Tensor orientation changes across this line, as will be detailed in subsequent steps.
Horizontal Distribution

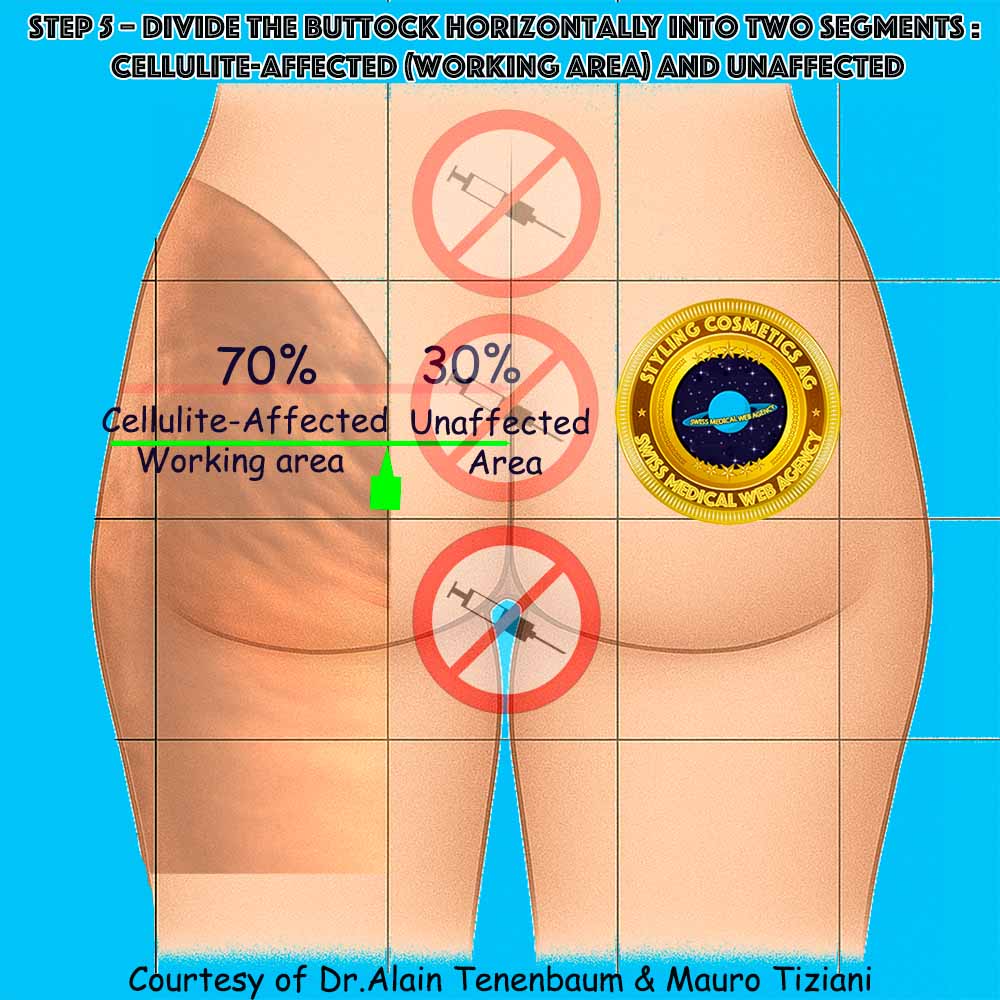
70%
External region – most commonly affected due to dense fibrous septa and mechanical stress.
20%
Central region – occasionally affected, with variable dimpling depending on morphotype.
10%
Internal region – usually spared, adjacent to the intergluteal cleft.

Grid-Based Division of the Gluteal Working Area
To standardize treatment planning, the cellulite-affected gluteal working area is first identified and then subdivided into a reproducible grid.
This approach ensures accuracy, symmetry, and homogeneous coverage before applying Endopeel.

Vertical division into columns
(inter-column spacing defined by tongue depressors)
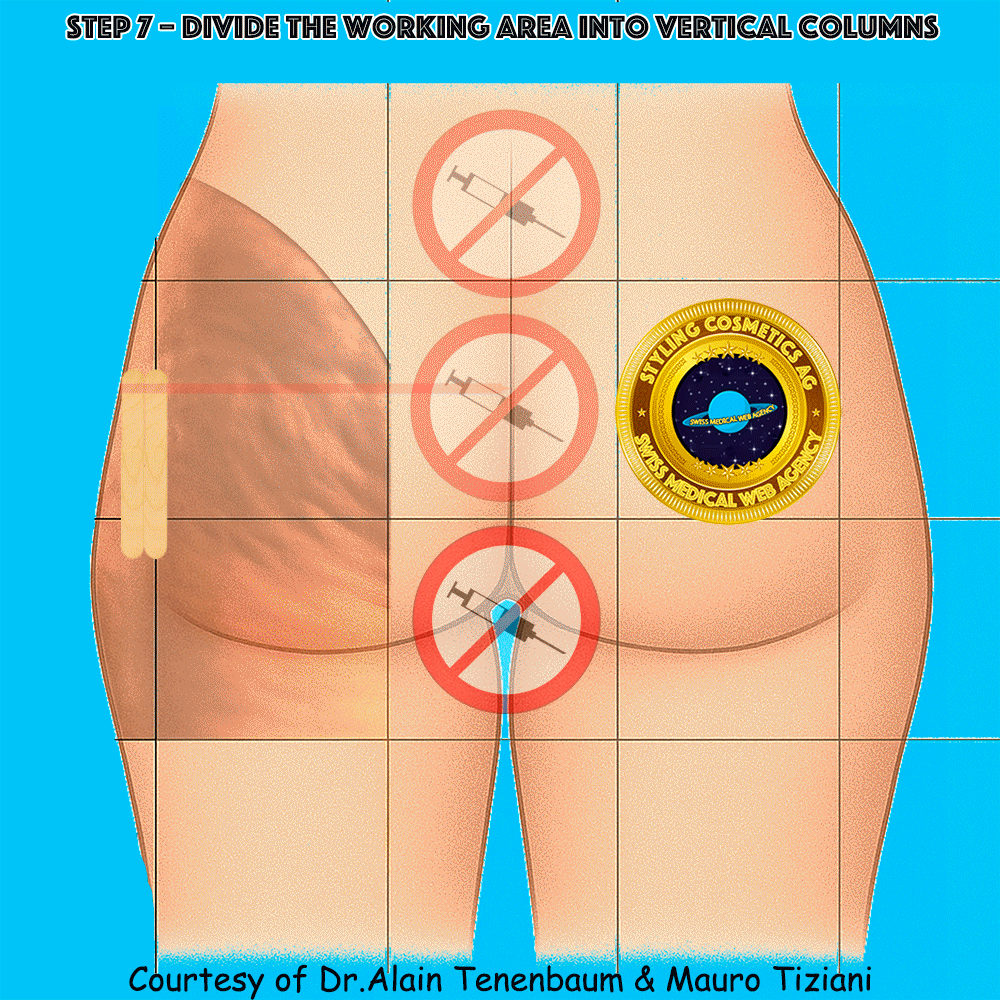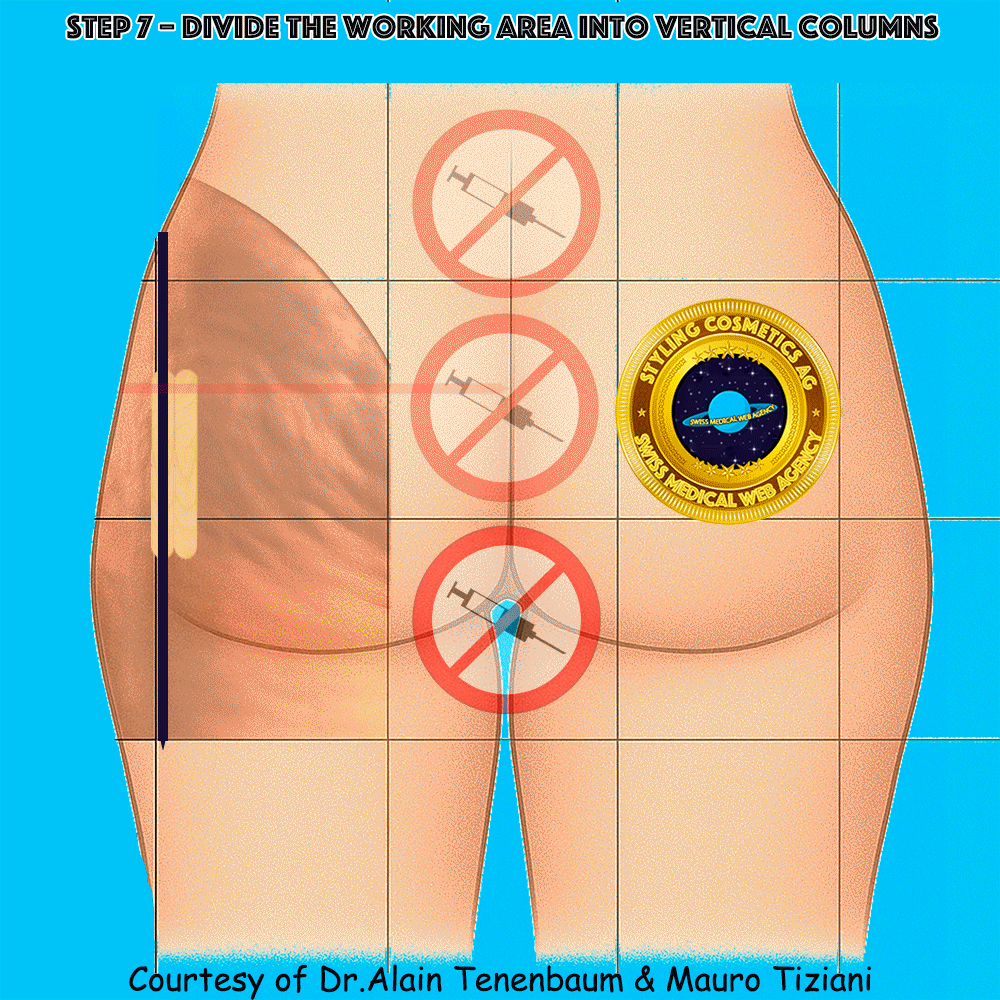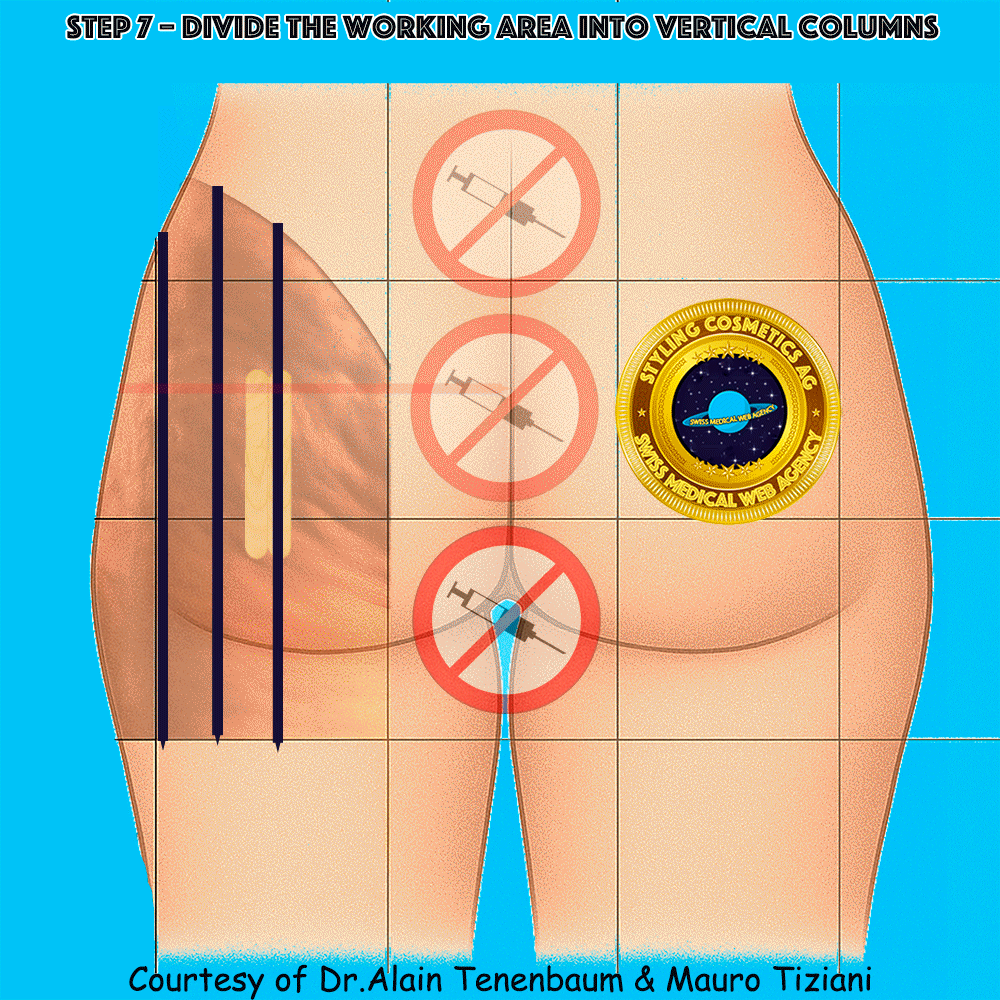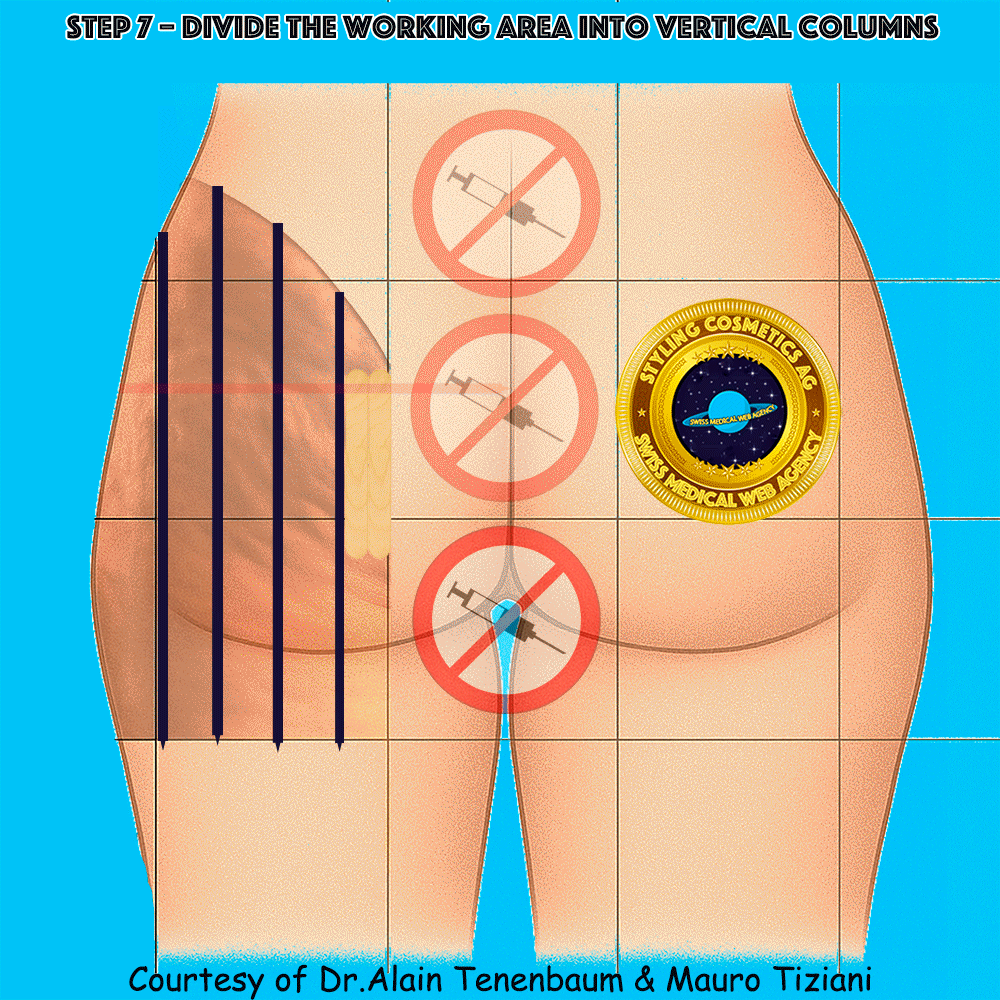
Horizontal division into rows
(inter-row spacing defined by tongue depressors)
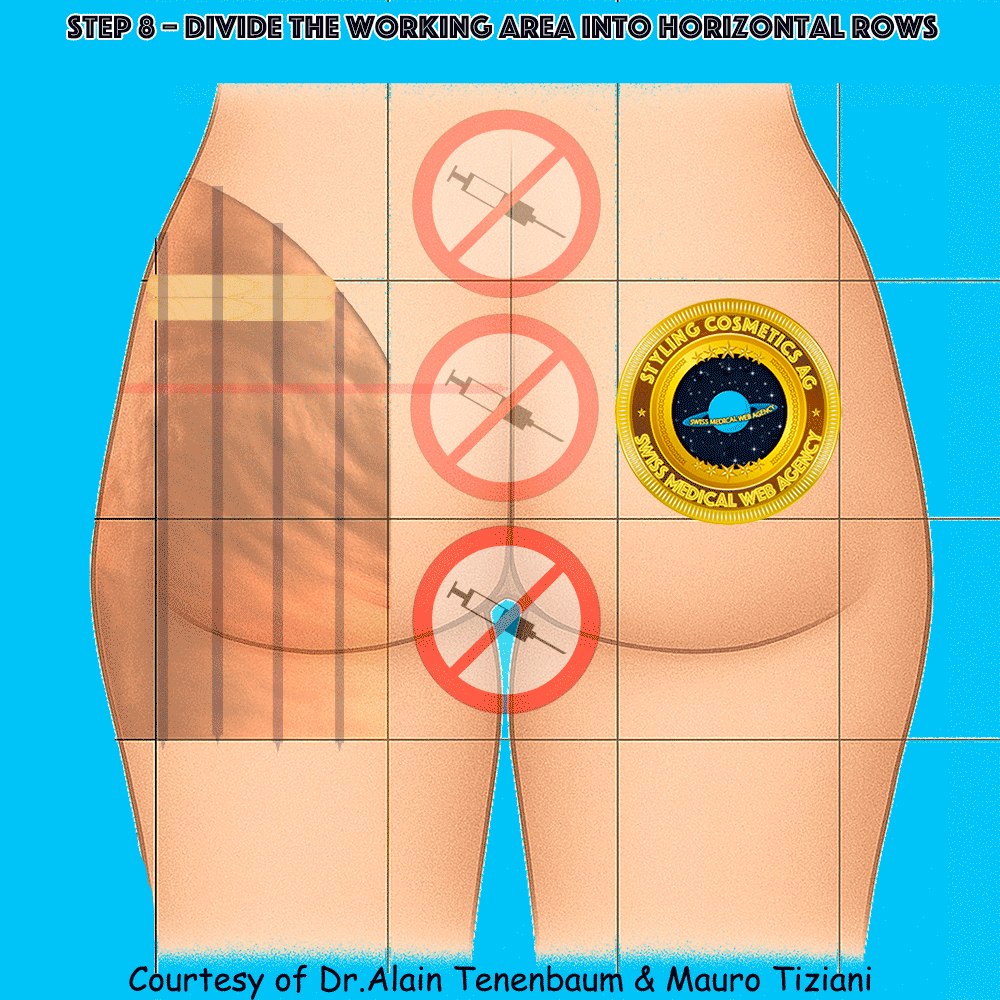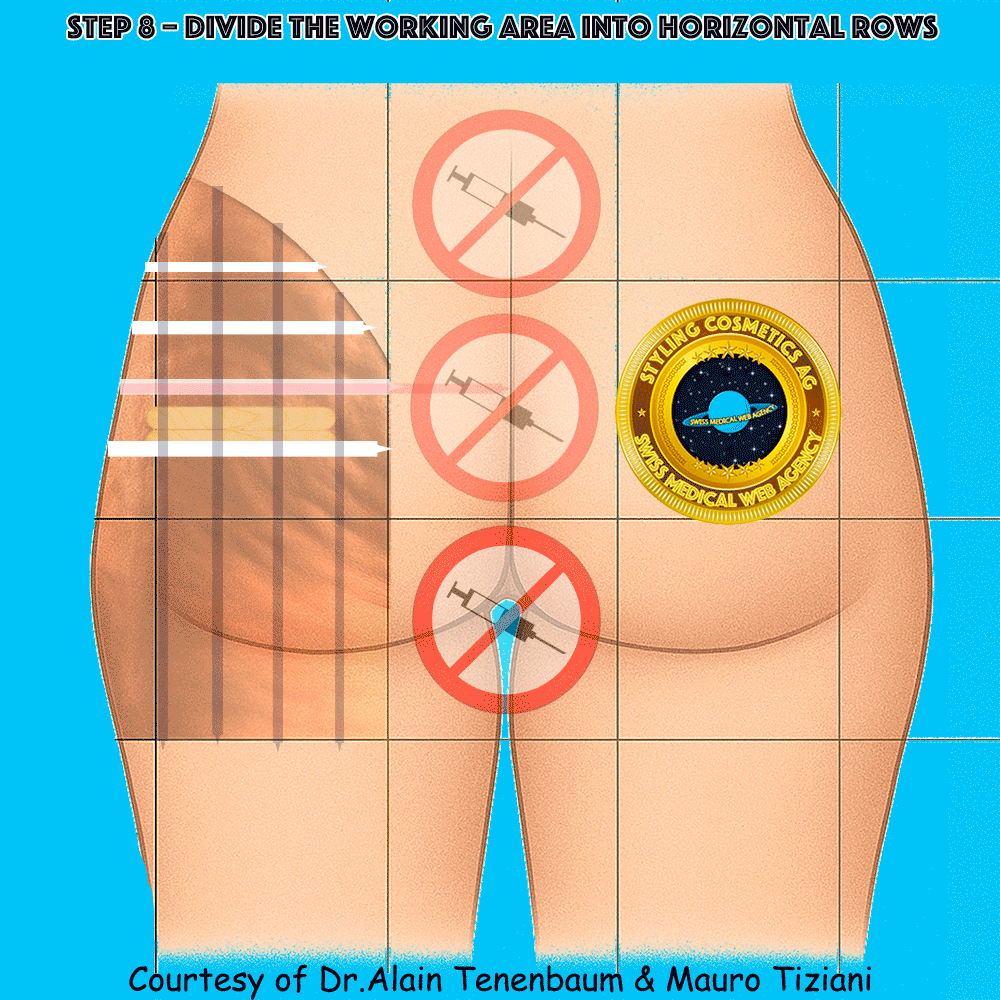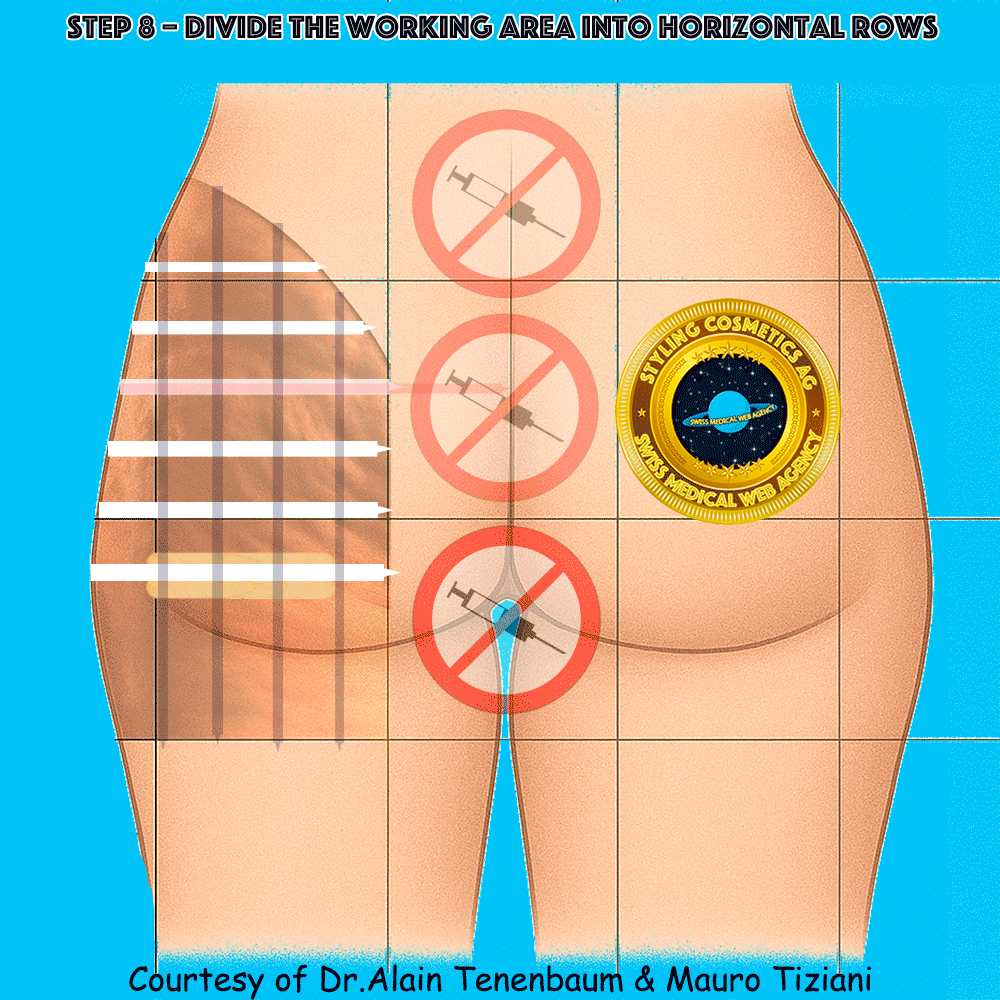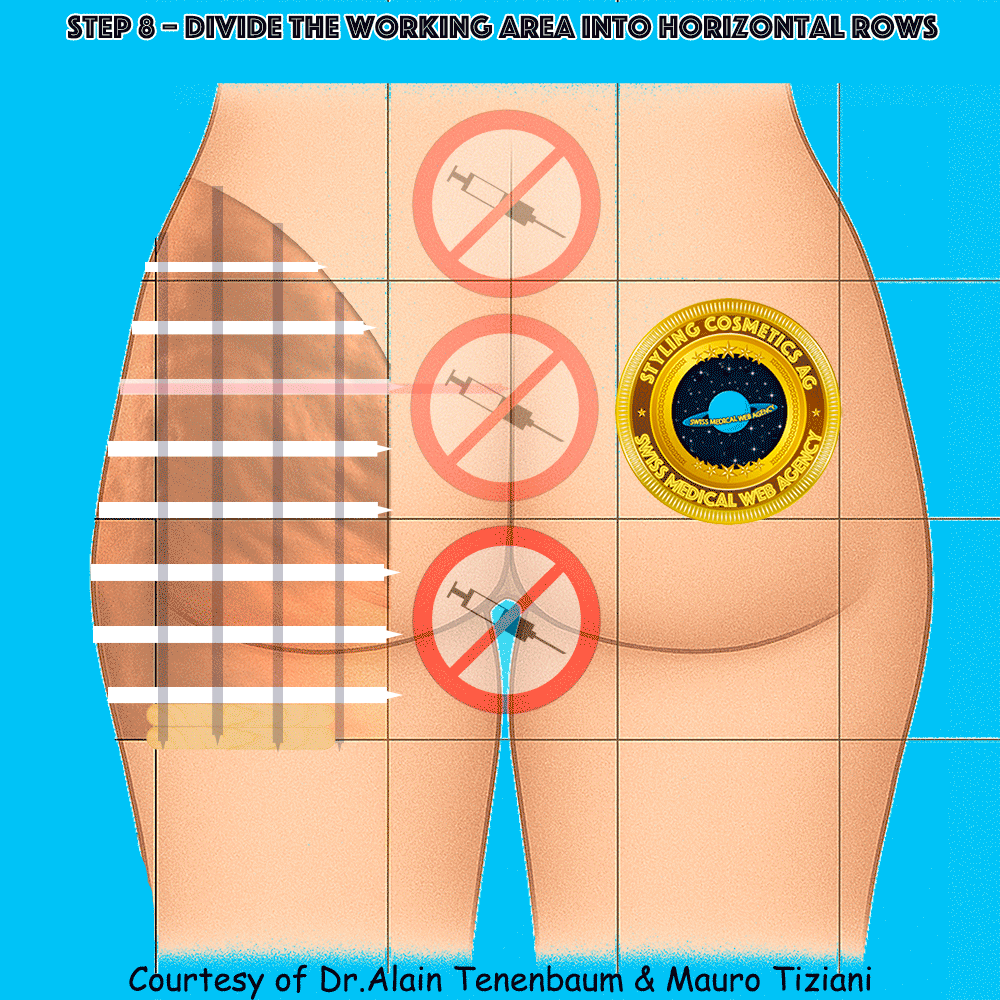
The intersection of columns and rows yields multiple treatment cells.
Each cell provides a reproducible reference for planning Endopeel interventions.

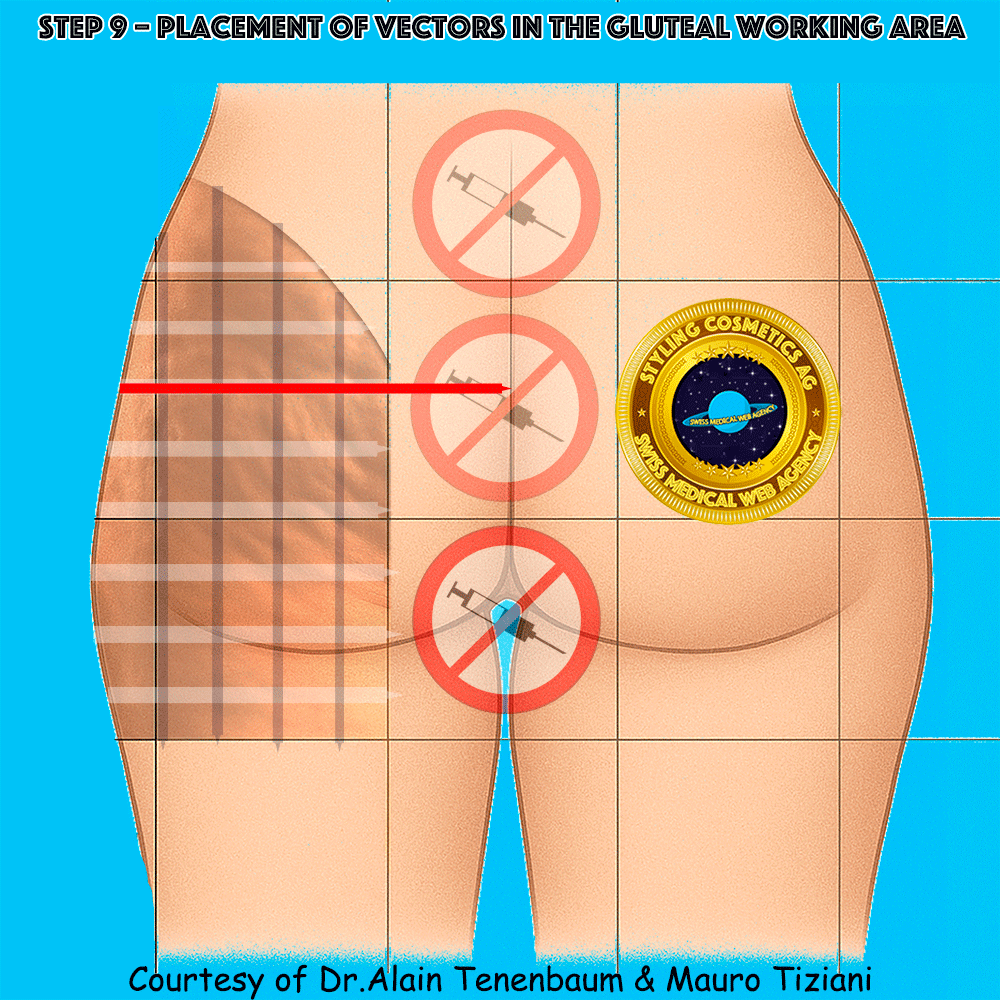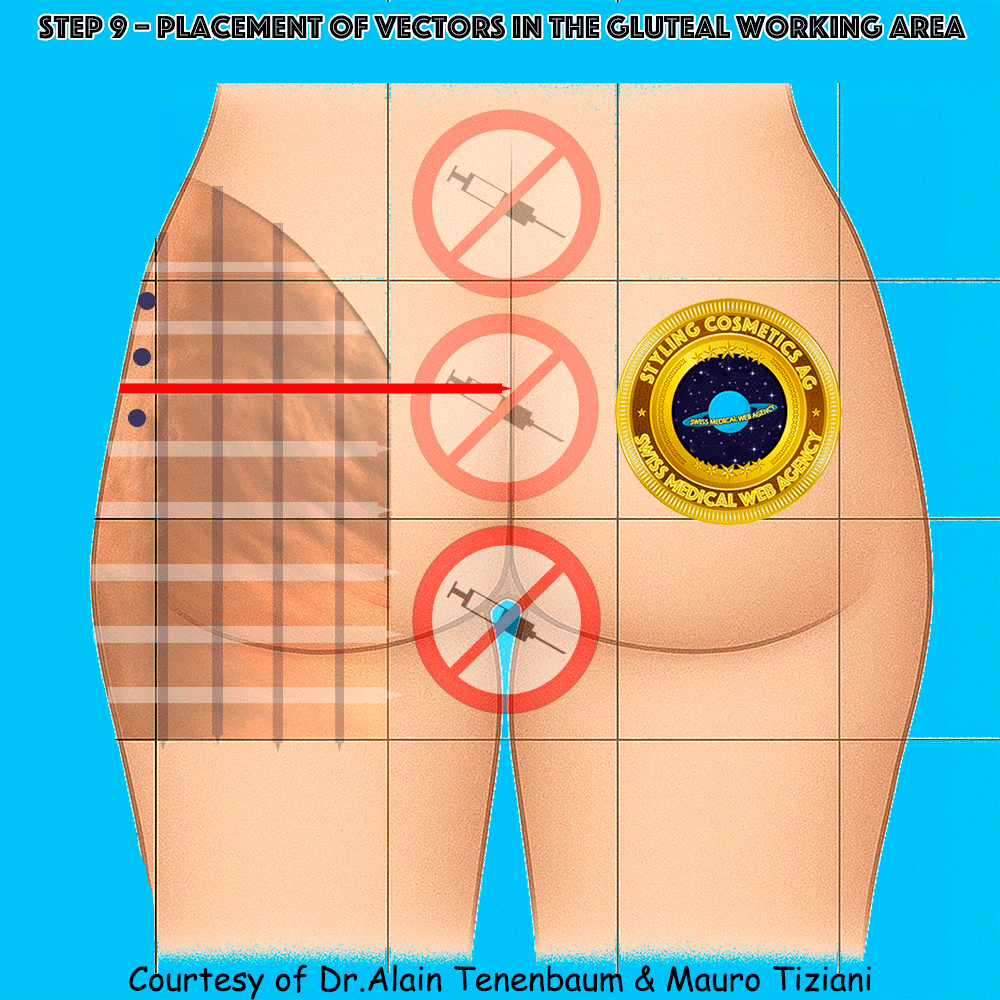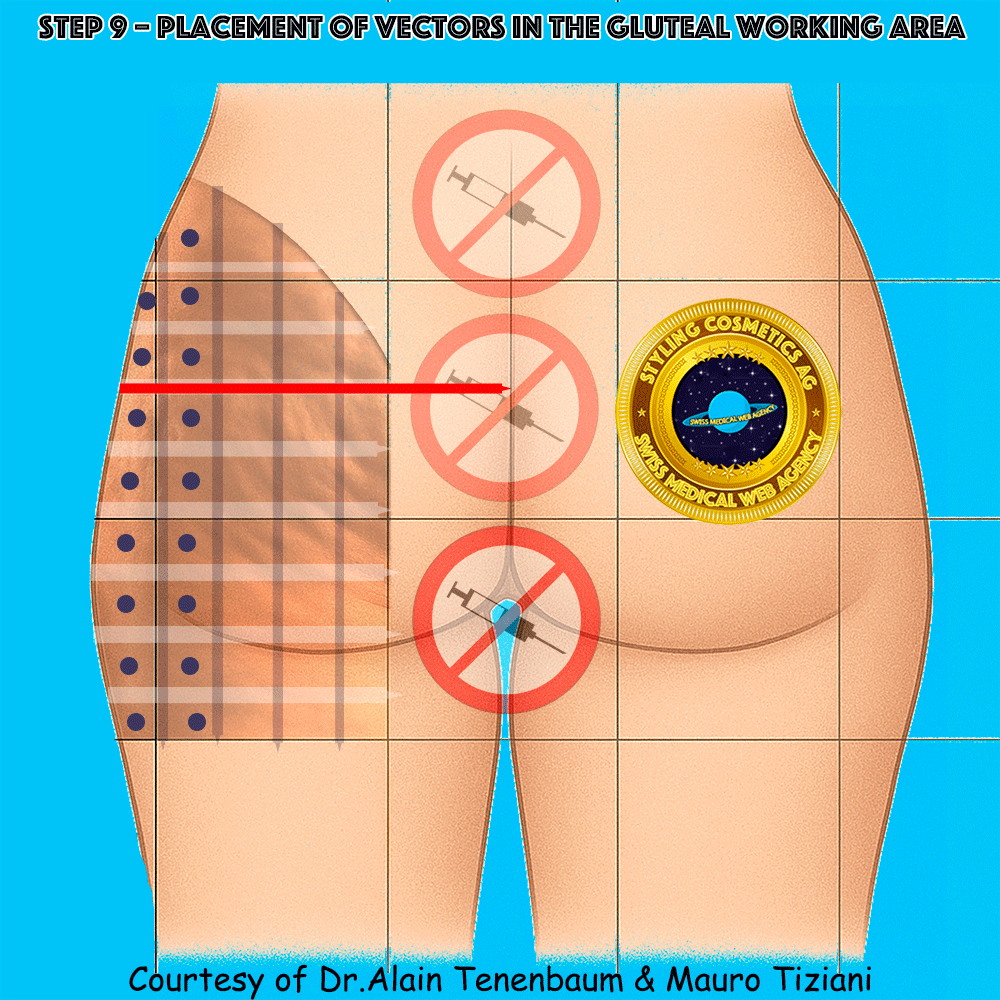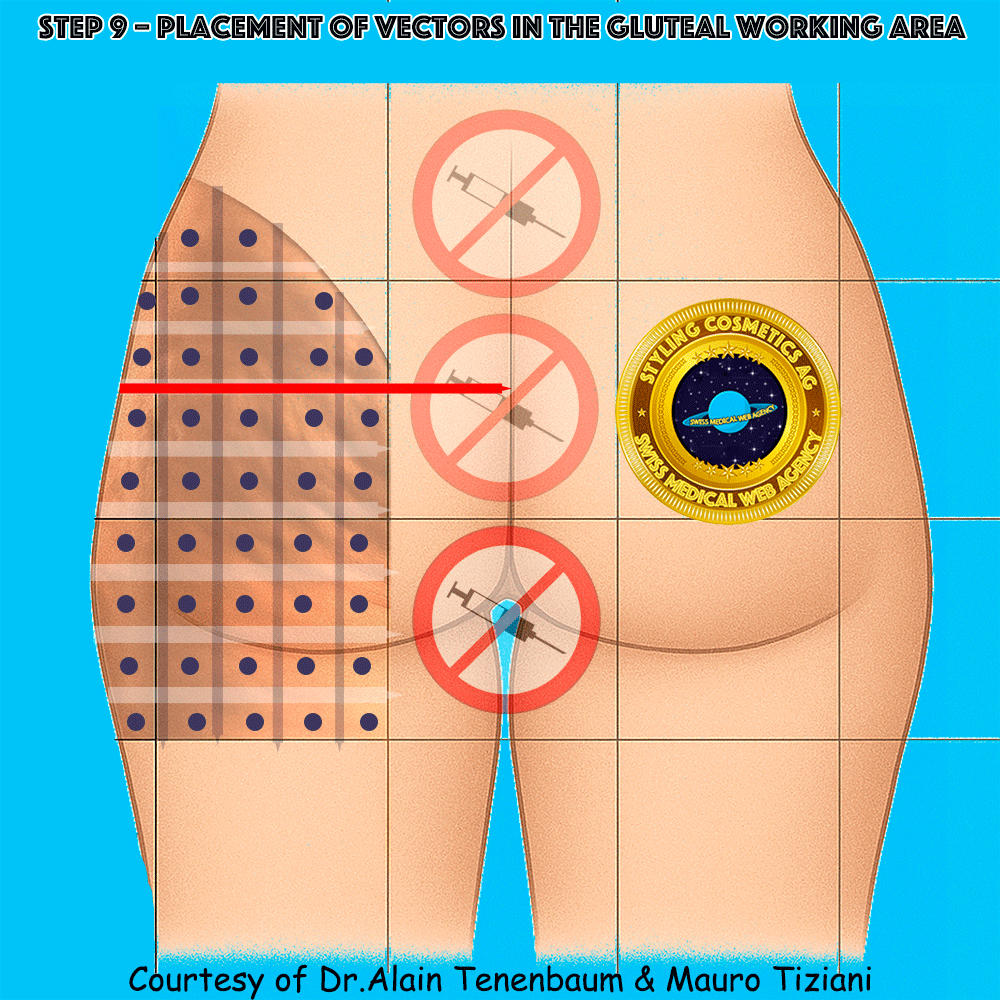
Placement of Vectors in the Gluteal Working Area
One vector per cell across the gluteal working area (blue ellipses denote vectors)
Injection Parameters
| Vector | Volume / Vector (mL) | Syringe | Needle |
|---|---|---|---|
| 1 vector / cell | 0.1 | 1 mL Luer-Lok (thick) | 27G flexible |
Needle Trajectory for Each Vector
Injection perpendicular to the cell surface at its center
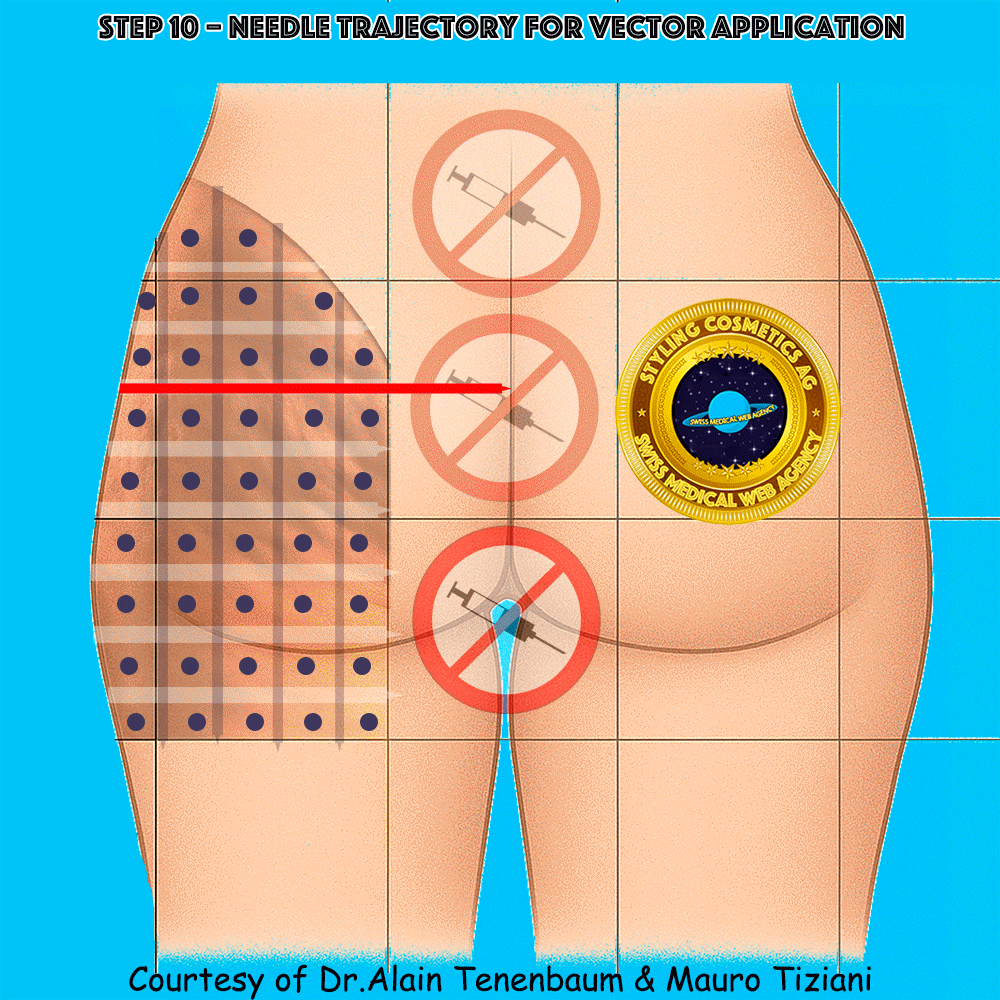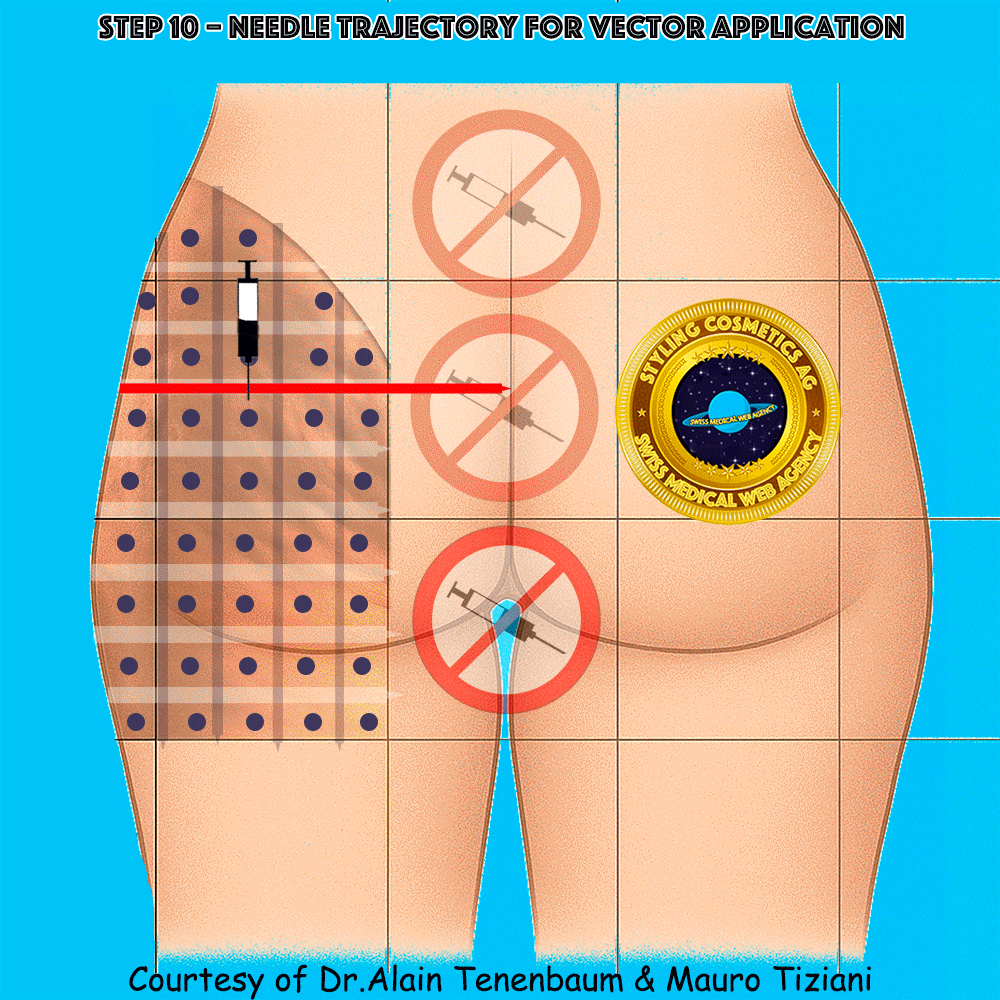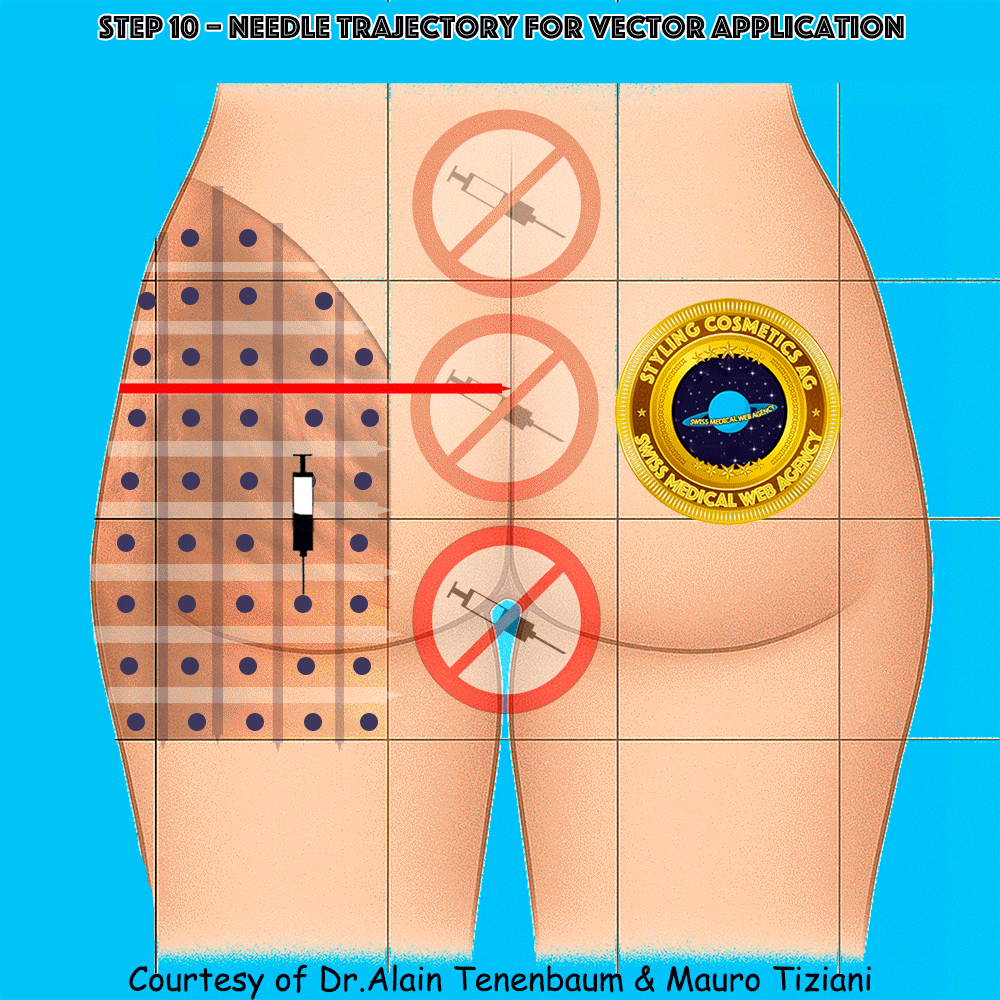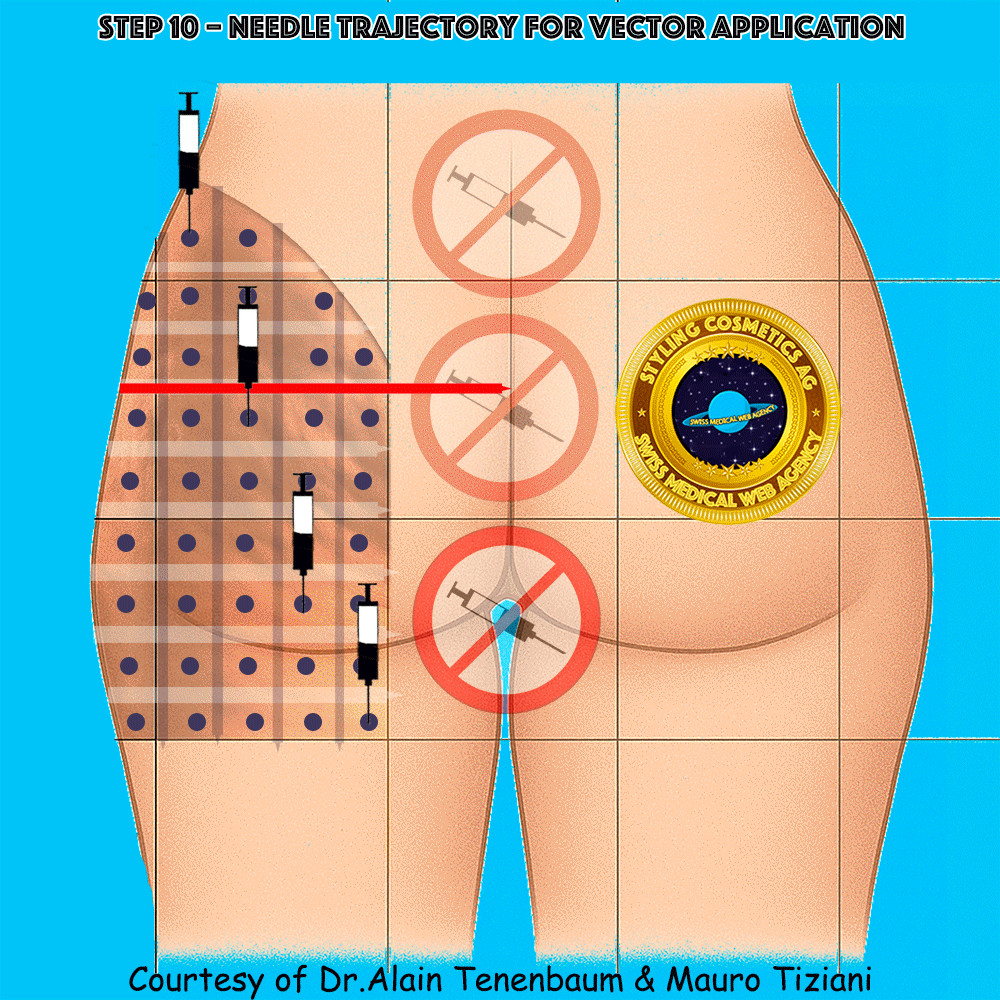
Trajectory & technique
| Vector | Volume / Vector (mL) | Syringe | Needle |
|---|---|---|---|
| 1 vector / cell | 0.1 | 1 mL Luer-Lok (thick) | 27G flexible |

Tensors — Placement & Needle Trajectory
Placement of tensors within the lower segment of the gluteal working area
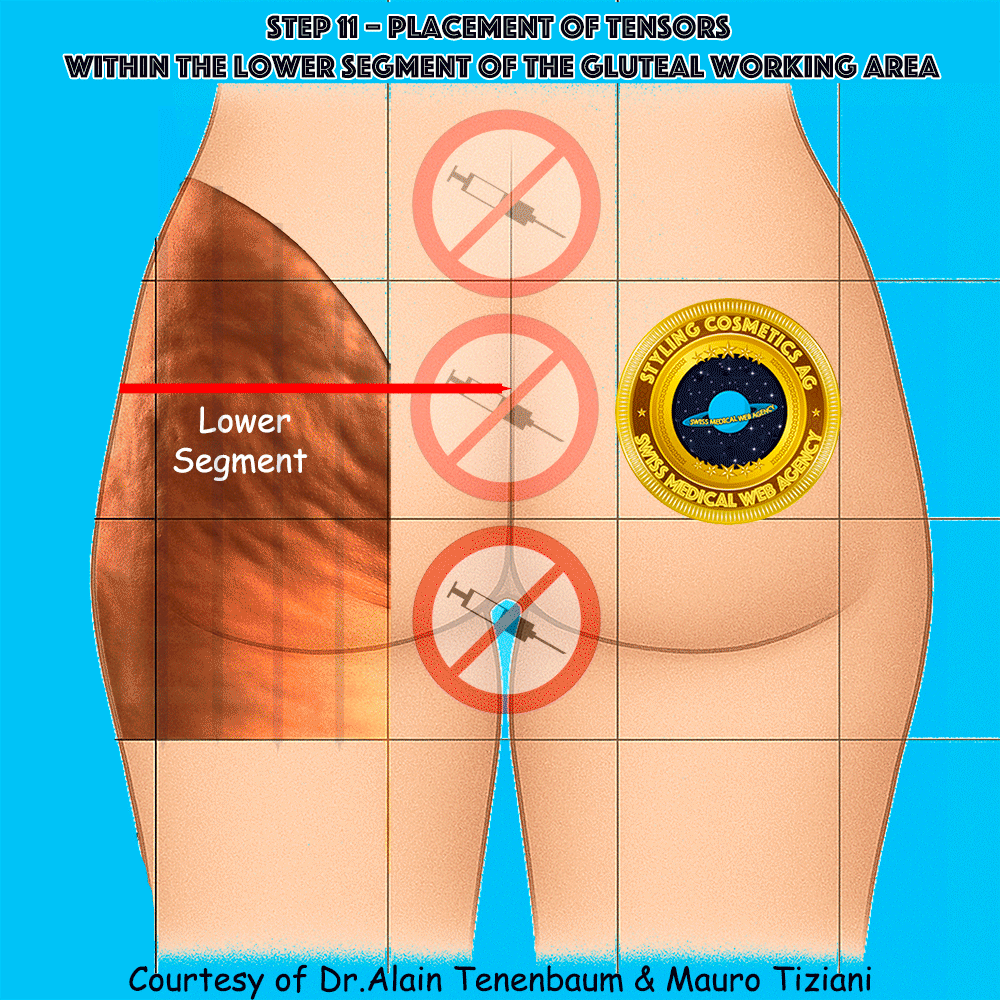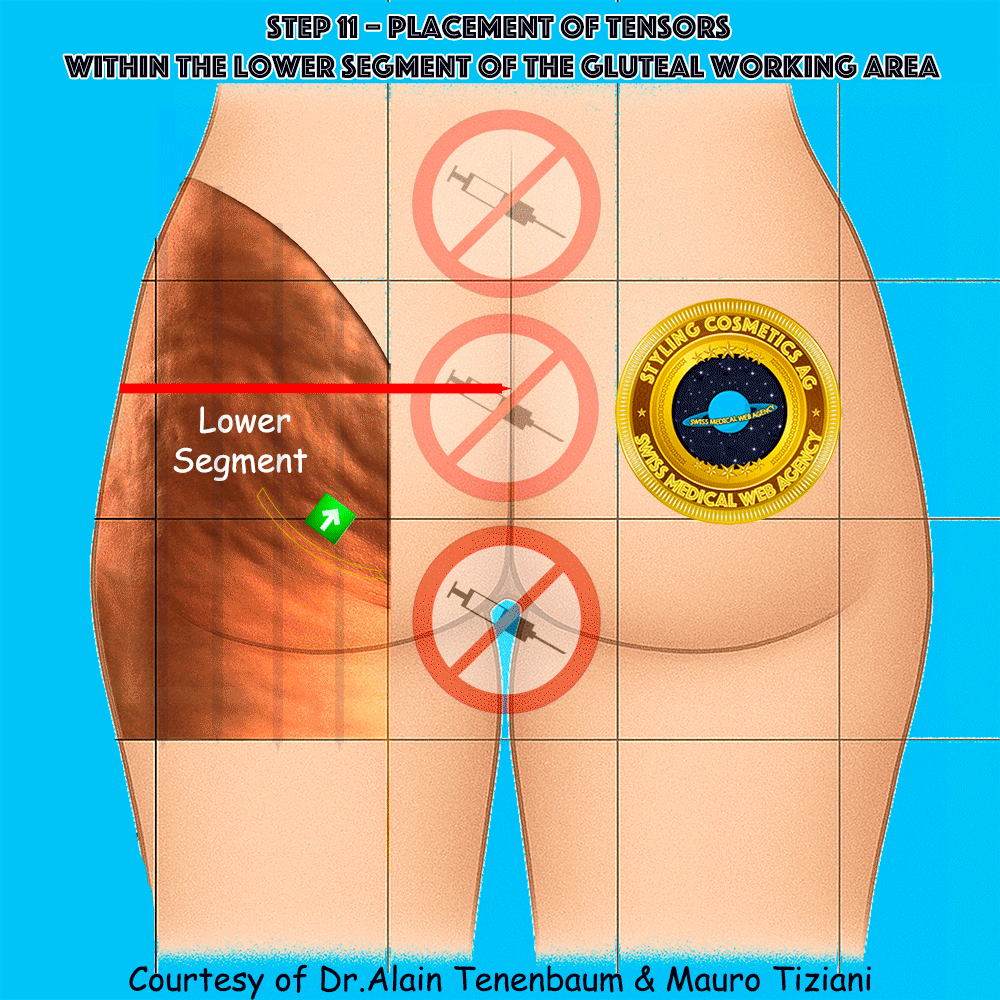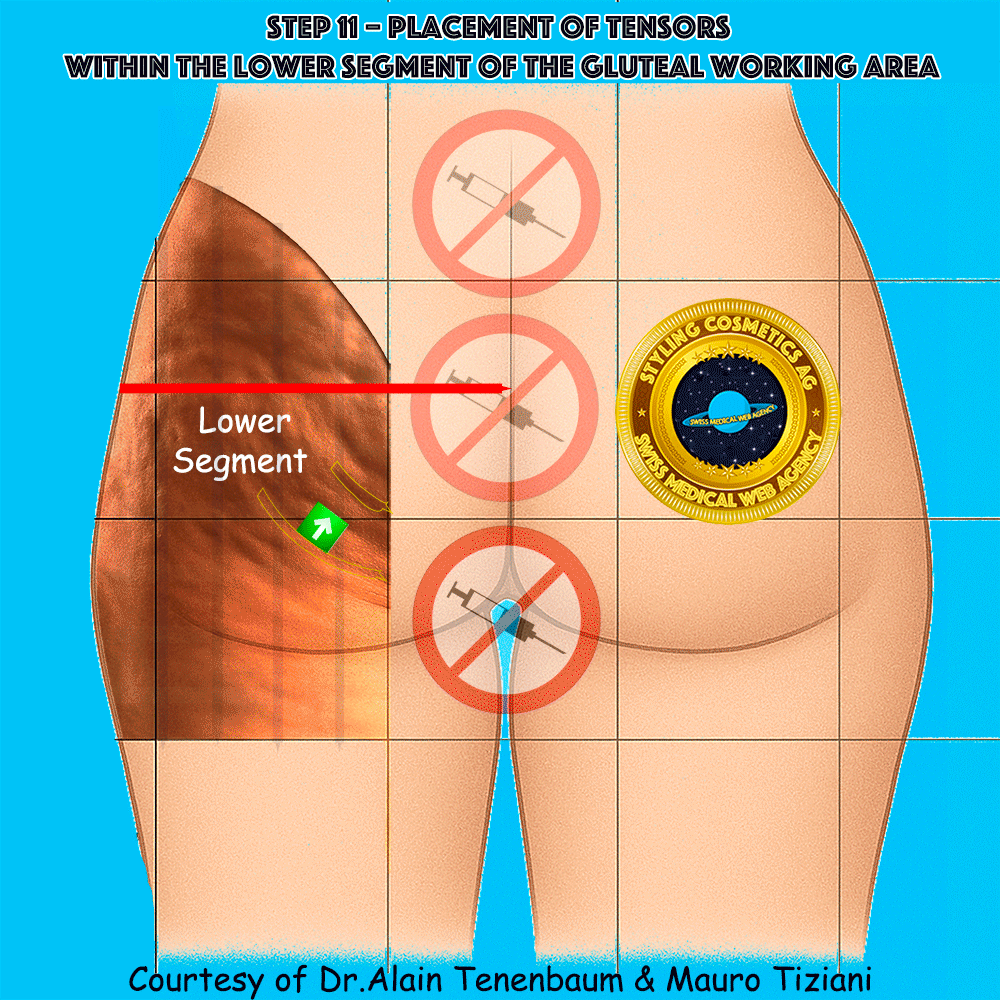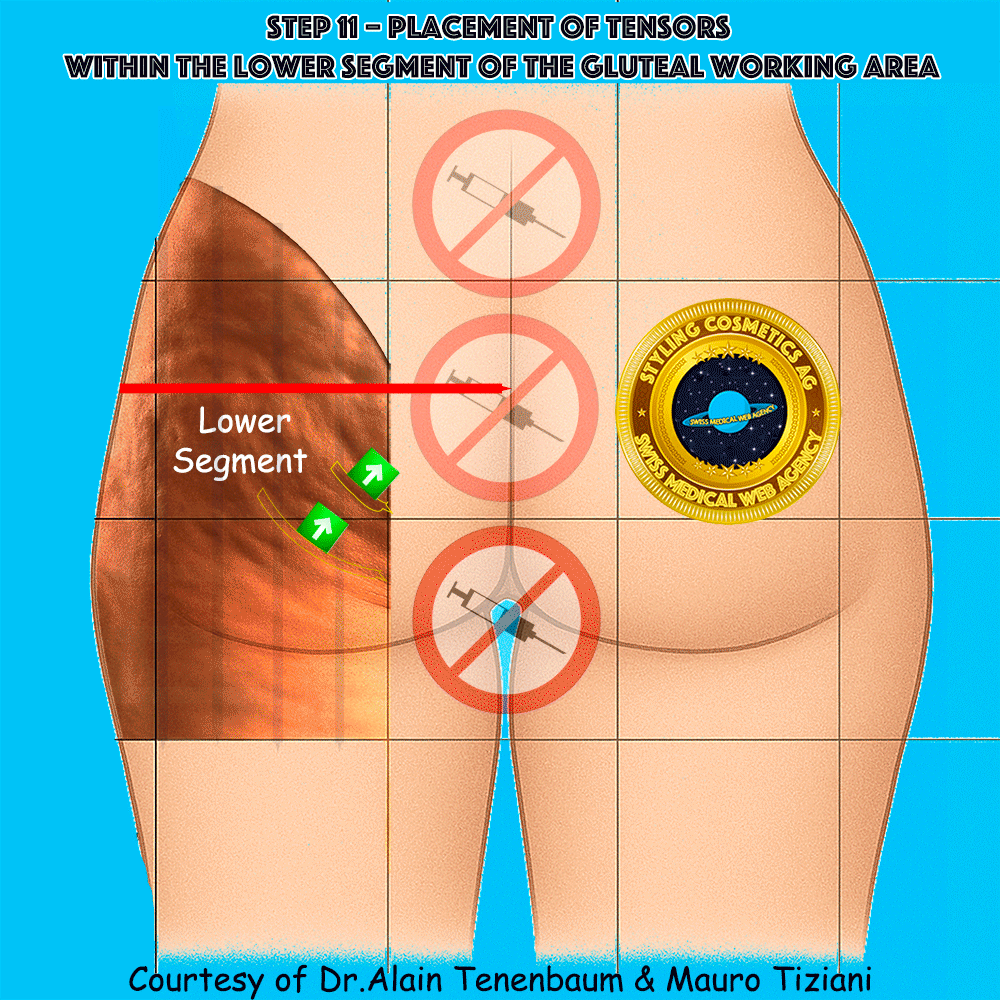
Unlike vectors, which are injected perpendicularly to the cell surface,
tensors are applied along the gluteal plane.
Each tensor must form a 90° angle with the selected fold of the cellulite cell,
ensuring effective mechanical action within the working area.
Needle trajectory for tensor application within the lower gluteal segment
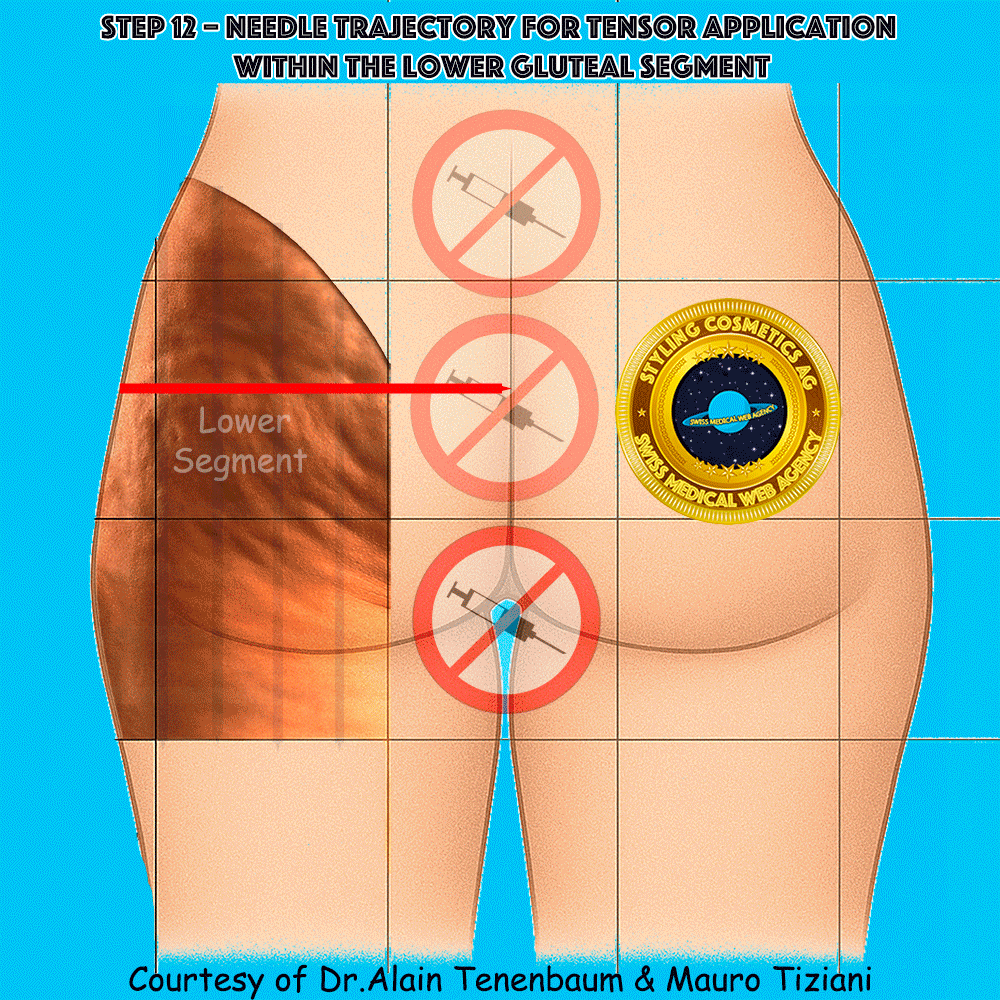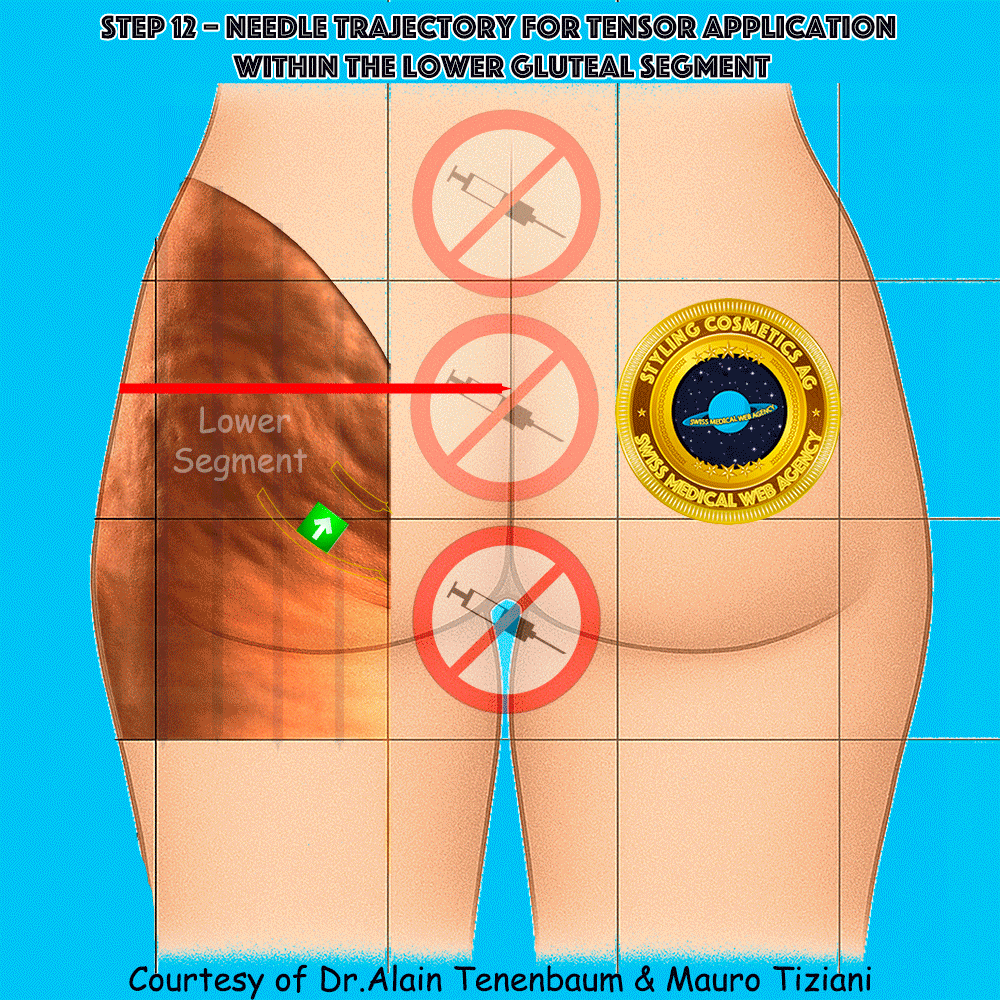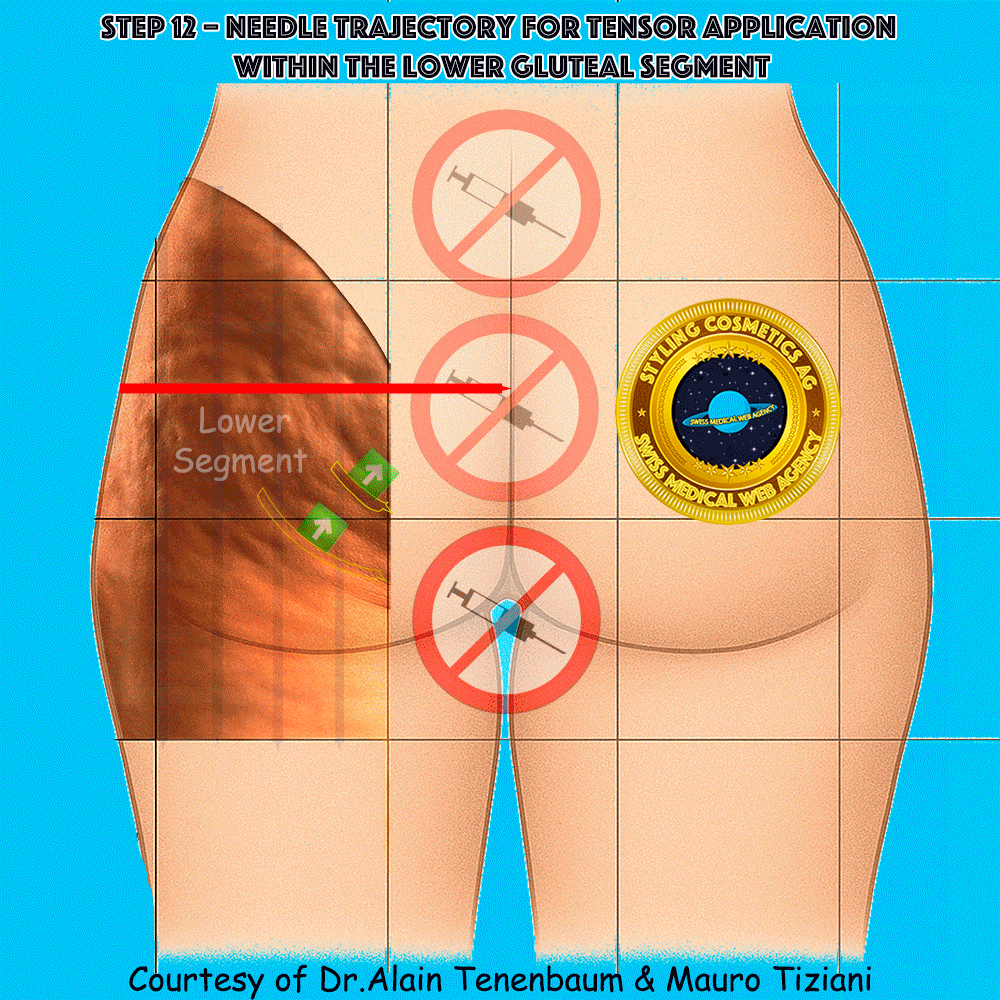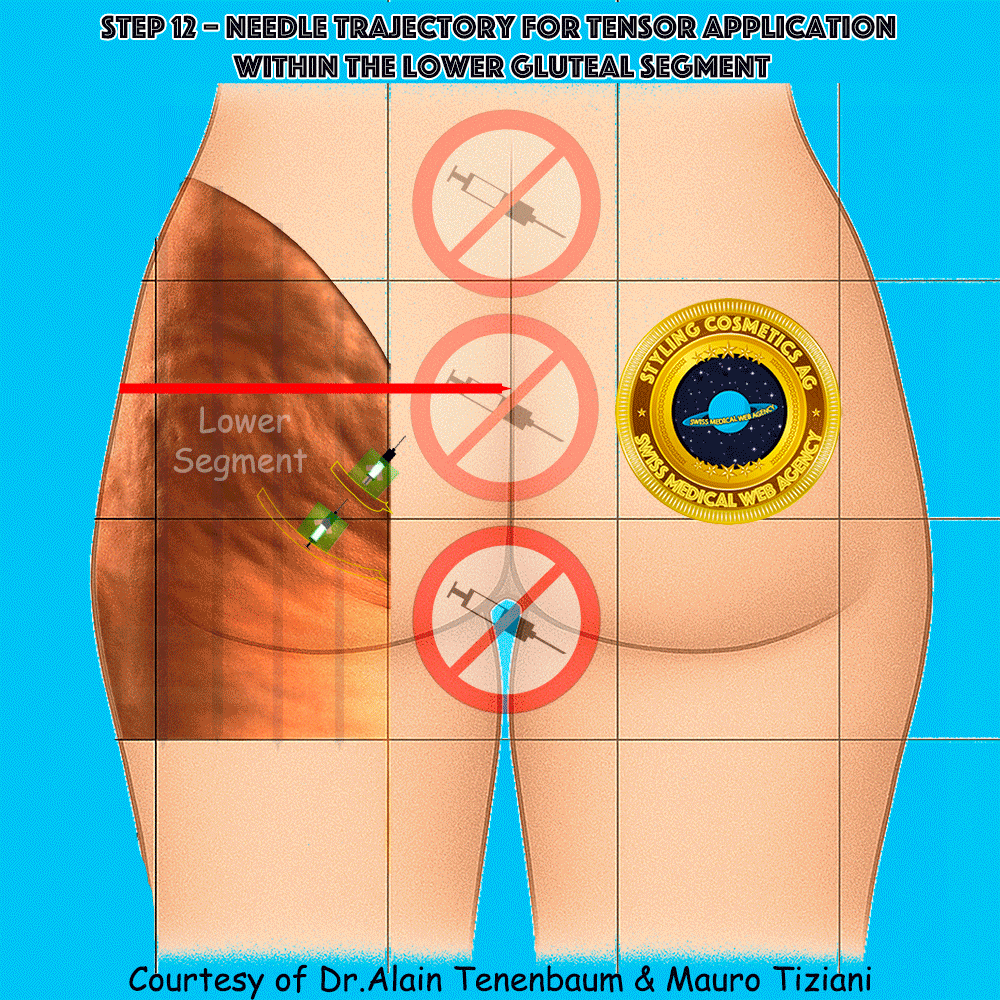
The syringe is applied directly along each tensor line (arrow). Injection must be performed without changing either the direction or the orientation of the tensor.
Placement of tensors within the upper segment of the gluteal working area
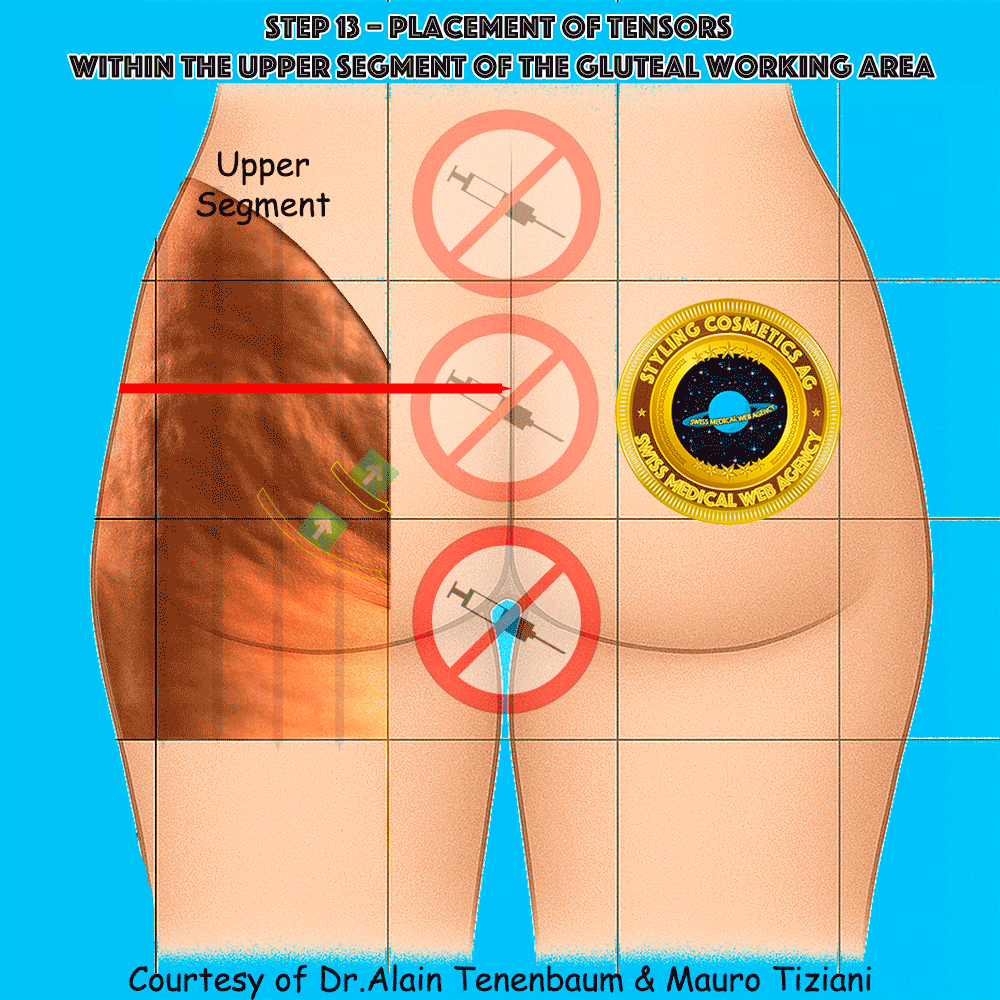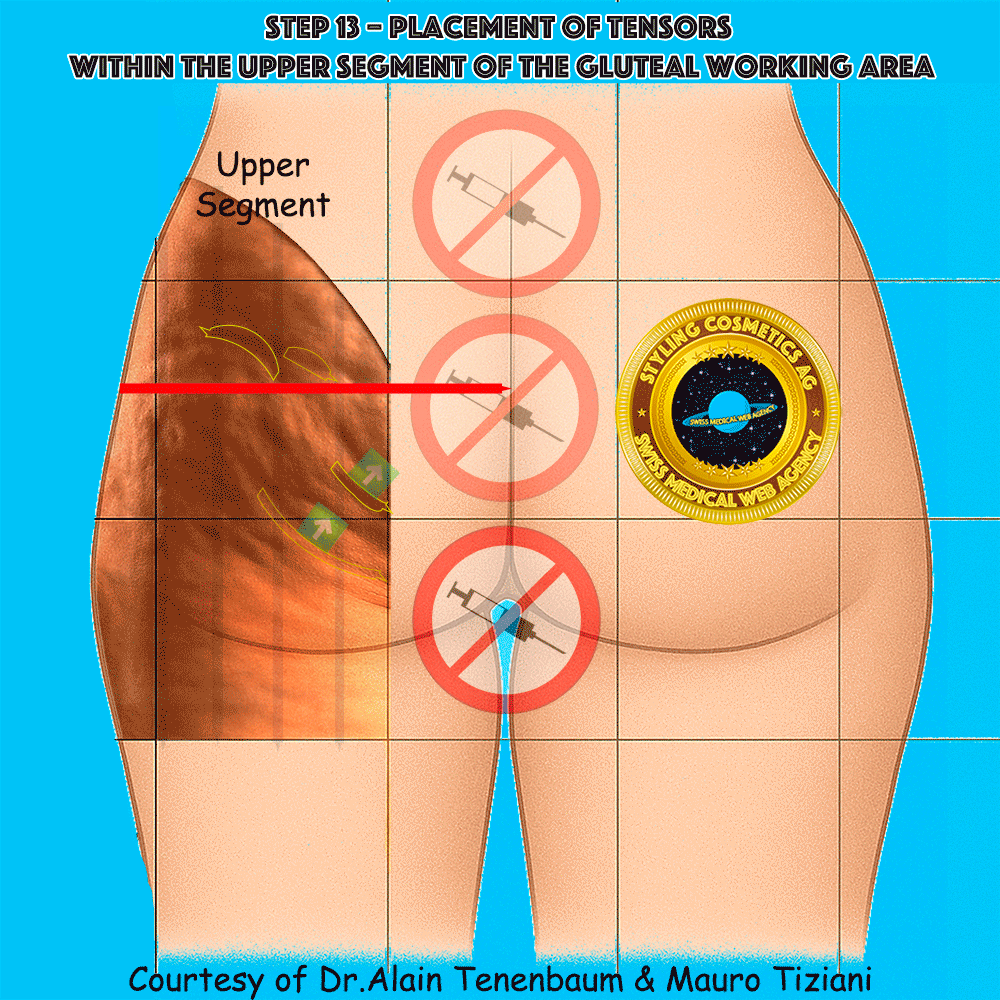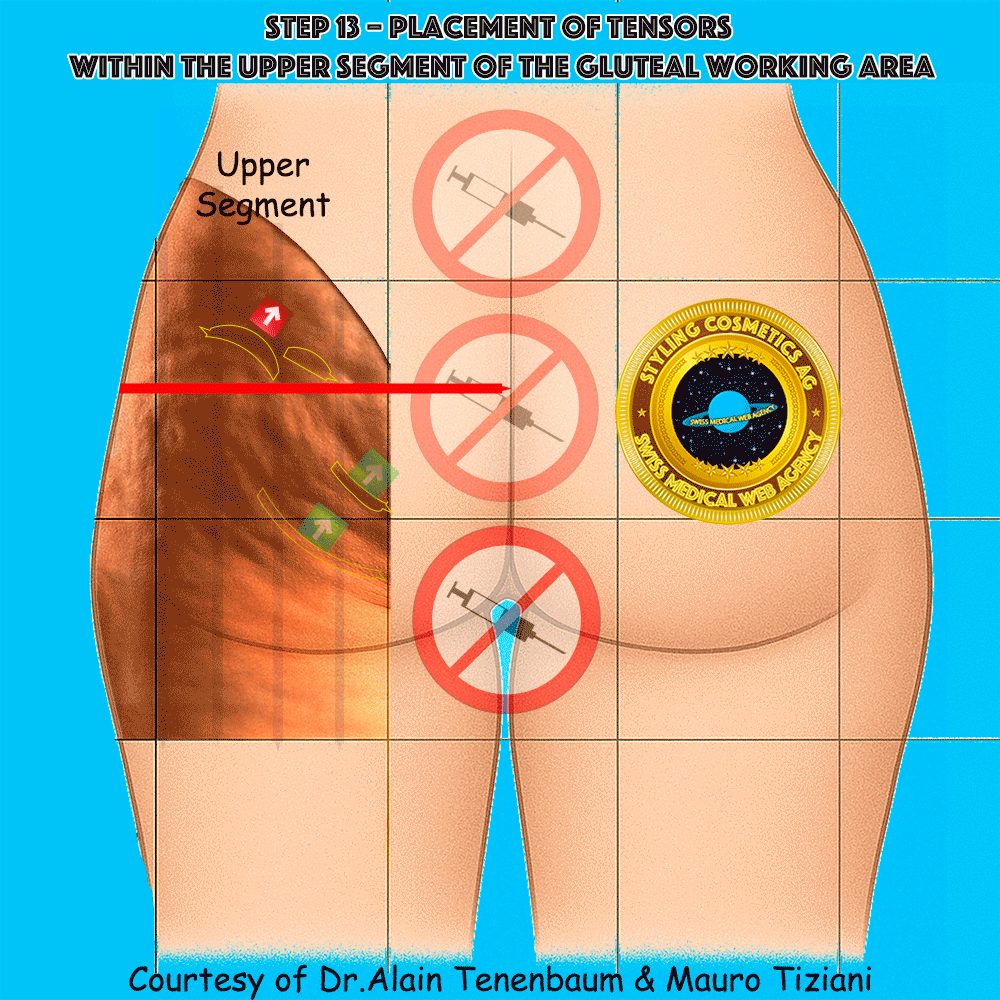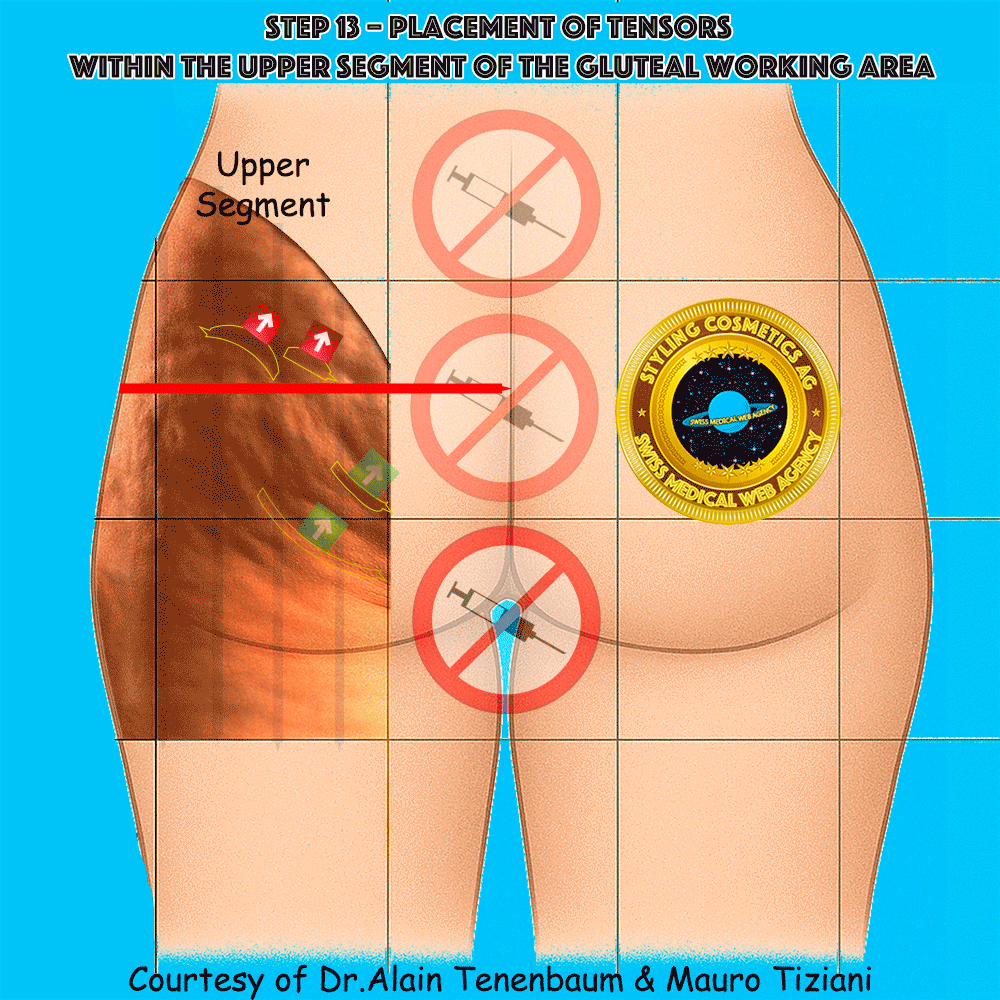
In the upper segment, cellulite folds often form an arc convex upward, whereas in the lower segment they typically form an arc concave upward. This distinction is clinically important, since the purpose of tensor application is to reduce the depth of these folds and restore a smoother contour
Needle trajectory for tensor application within the upper gluteal segment
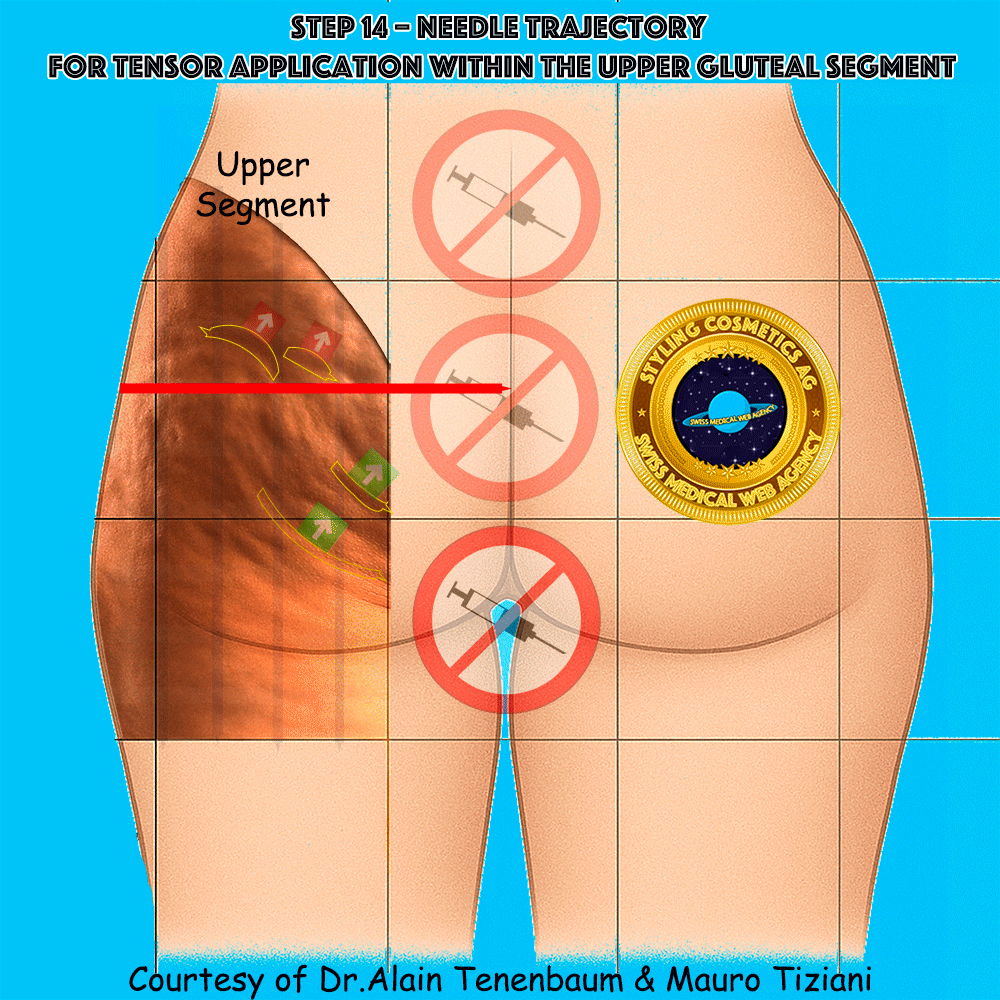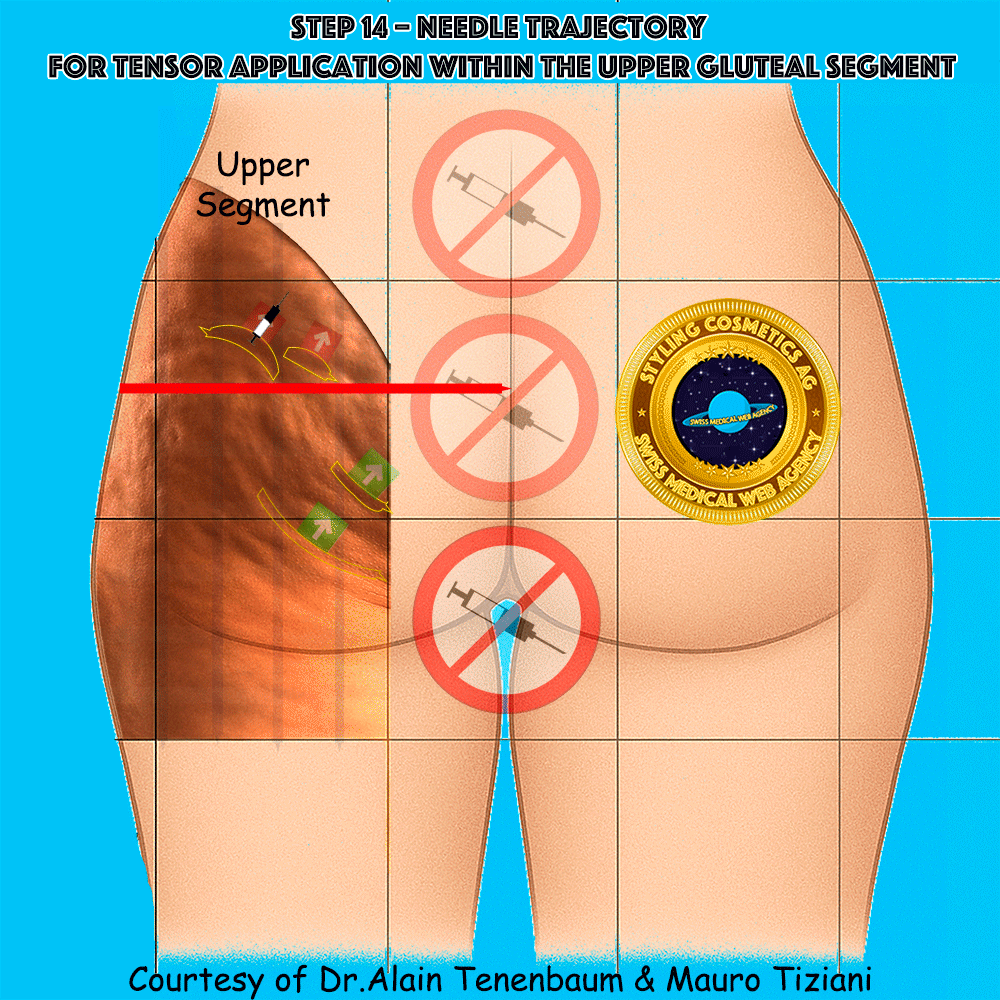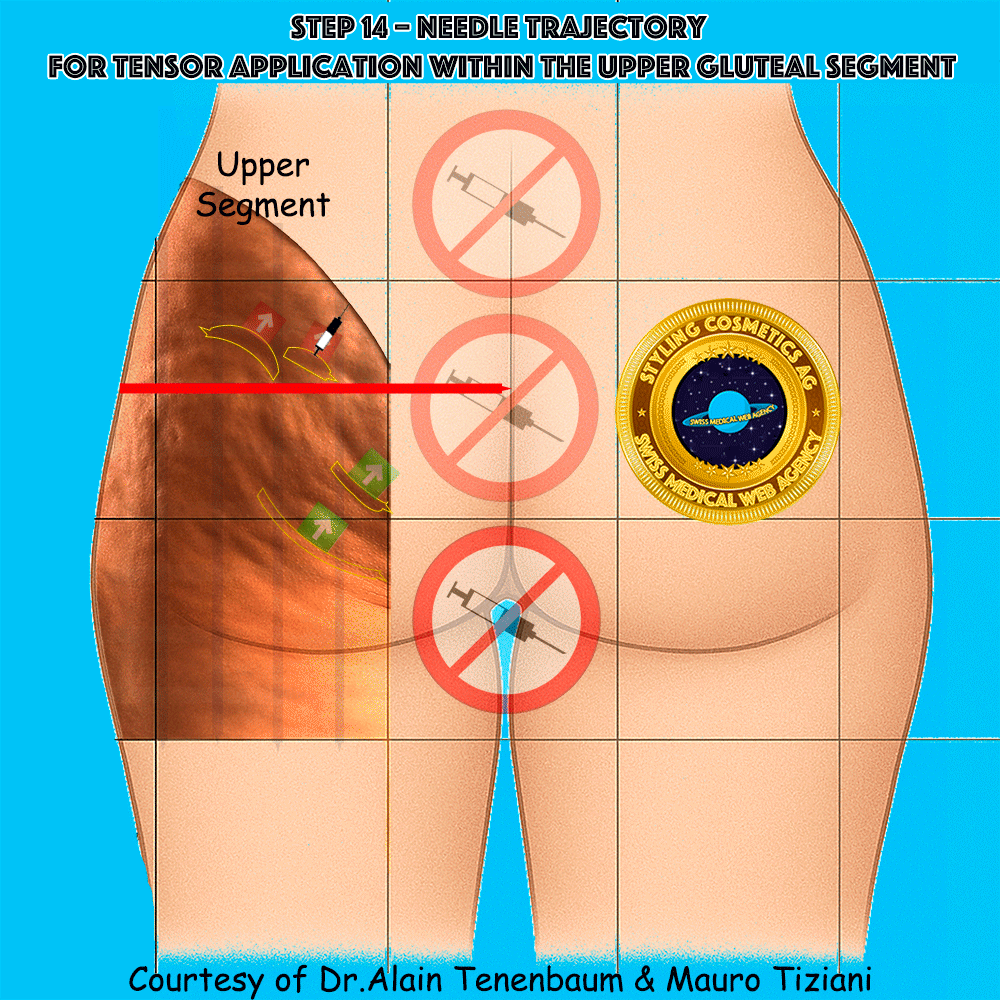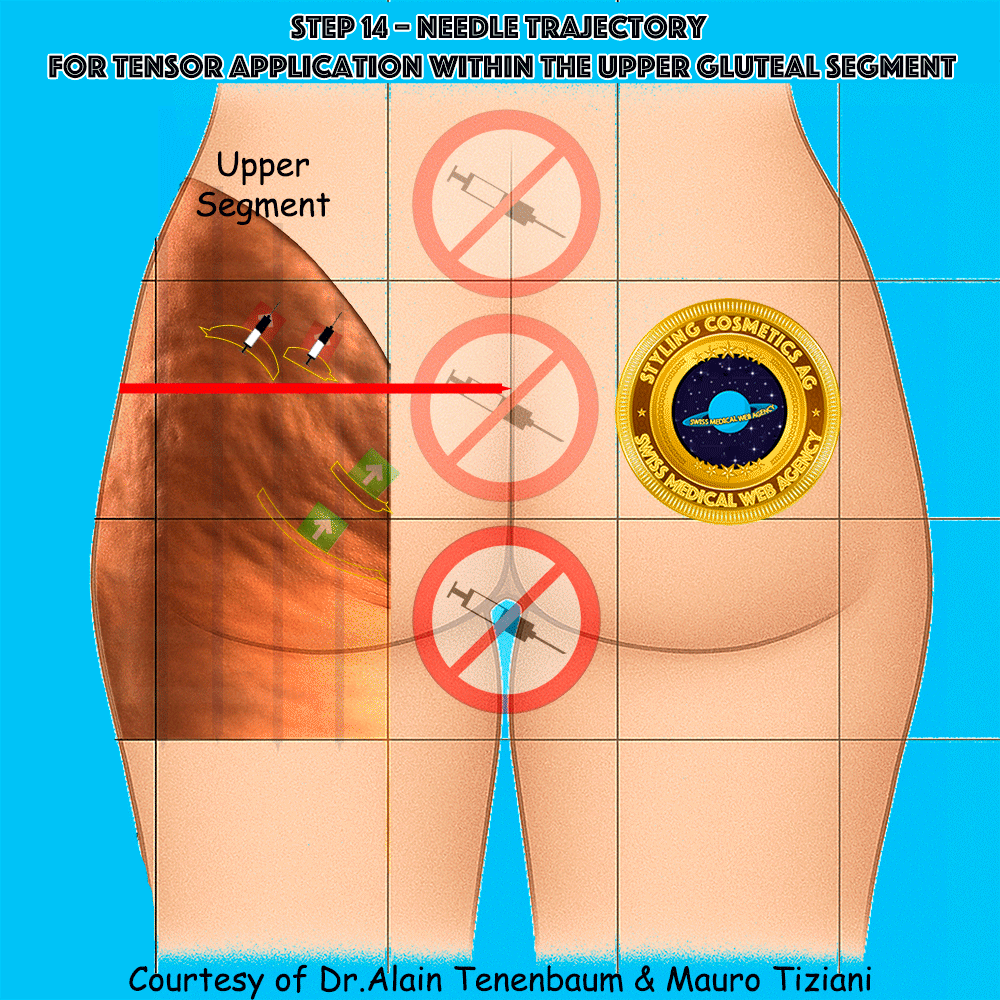
The syringe is applied along each tensor line in the upper segment.
Injection must follow the arrow without altering the planned direction,
so that the convex cellulite folds are progressively flattened
and their depth minimized.
| Syringe | Needle | Position | Quantity (mL) |
|---|---|---|---|
| 1 mL Luer-Lok (thick) | 27G flexible | Superficial subdermal plane | 0.1 per tensor |

Clinical Summary
This standardized grid‑based technique enables reproducible planning and execution of gluteoplasty with Endopeel. By systematically combining vectors and tensors, symmetry, safety, and clinical predictability are optimized.
Key Parameters
- One vector + one tensor per cell, 0.1 mL each
- Syringe: 1 mL Luer-Lok (thick)
- Needle: 27G flexible
- Planes: Vectors — superficial subdermal to intramuscular (per training protocol); Tensors — superficial subdermal, tangent to the gluteal plane, oriented 90° to the selected fold
- Strict adherence to Endopeel training protocols
Further Information
Access essential guidance for safe and effective practice.
■ Gluteoplasty for cellulite reduces dimpling only.
■ 3D gluteal reshaping modifies contour and projection.
■ Sequence: cellulite first; then a second session (15–30 days) for 3D reshaping if desired.
■ Inform patients: the two procedures are distinct but complementary.
■ Other areas: cellulite may also involve thighs, arms, and abdomen.

